Cilostazol for Poor Circulation: What It Really Does and When to Use It
Cilostazol is often described as one of the most effective medications for poor circulation in the legs—but what does it actually do? Does it dissolve clots in your veins? Can it clear blocked arteries overnight? Understanding what this drug is designed for, how it works, and when it should not be used is essential for staying safe and getting real benefits.
If you live with poor circulation, you know how limiting it can be. Even a short walk may trigger pain and force you to stop. Cilostazol, marketed under brand names such as Pletal, is commonly prescribed to help people in this situation.
In this guide, based on the insights of Dr. Antonio Cascelli, we’ll explain:
- How Cilostazol helps with blocked arteries in the legs
- Why it is not a treatment for vein problems like varicose veins
- How it fits into a broader plan for managing arterial disease
- The main precautions and side effects you need to know
Think of this as a clear, practical overview of one of the key medications used in peripheral artery disease (PAD).
Key Takeaways
-
Cilostazol targets arteries, not veins
It is used to treat poor circulation caused by blocked arteries (atherosclerosis), especially in the legs. It is not meant for varicose veins or deep vein thrombosis (DVT). -
It helps you walk farther with less pain
Cilostazol improves walking distance in people with intermittent claudication—leg pain caused by narrowed arteries during activity. -
How it works
Cilostazol acts as a vasodilator (it widens blood vessels) and also has antiplatelet effects (it makes blood platelets less likely to clump), improving blood flow in narrowed arteries. -
It’s only one part of treatment
Cilostazol supports a broader plan that must include lifestyle changes (diet, exercise, quitting smoking) and other essential medications to manage blood pressure, cholesterol, and diabetes. -
It requires medical supervision
Cilostazol can cause side effects and is not safe for everyone, especially some patients with heart problems. It should only be used under a healthcare provider’s guidance.
1. What Is Poor Arterial Circulation? Atherosclerosis in Plain Language
To understand why Cilostazol is prescribed, you first need to understand atherosclerosis, the condition it is designed to help manage.
Your arteries are flexible tubes that carry oxygen-rich blood from the heart to the rest of the body. In a healthy person, these vessels are smooth and wide open, allowing blood to flow freely.
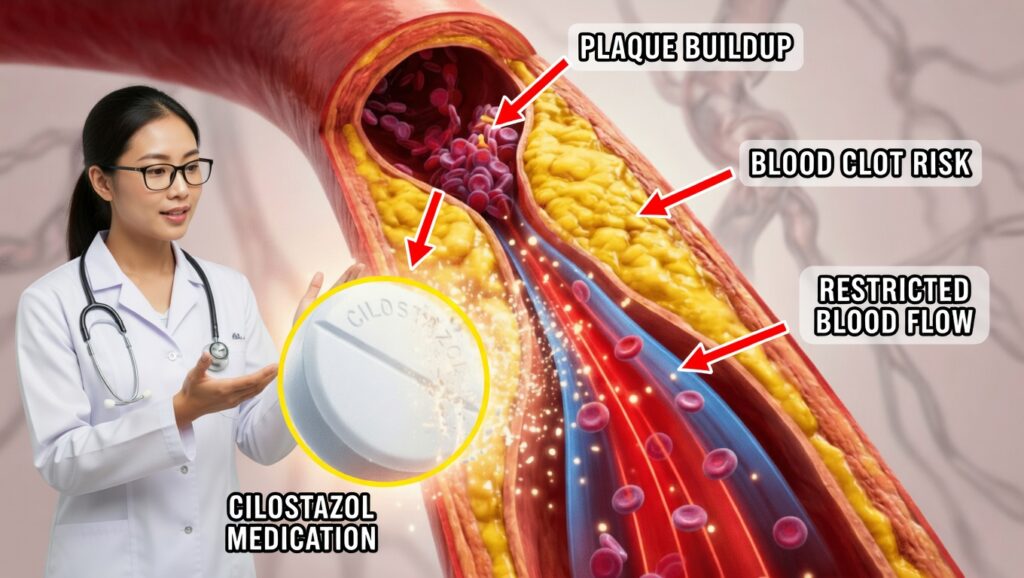
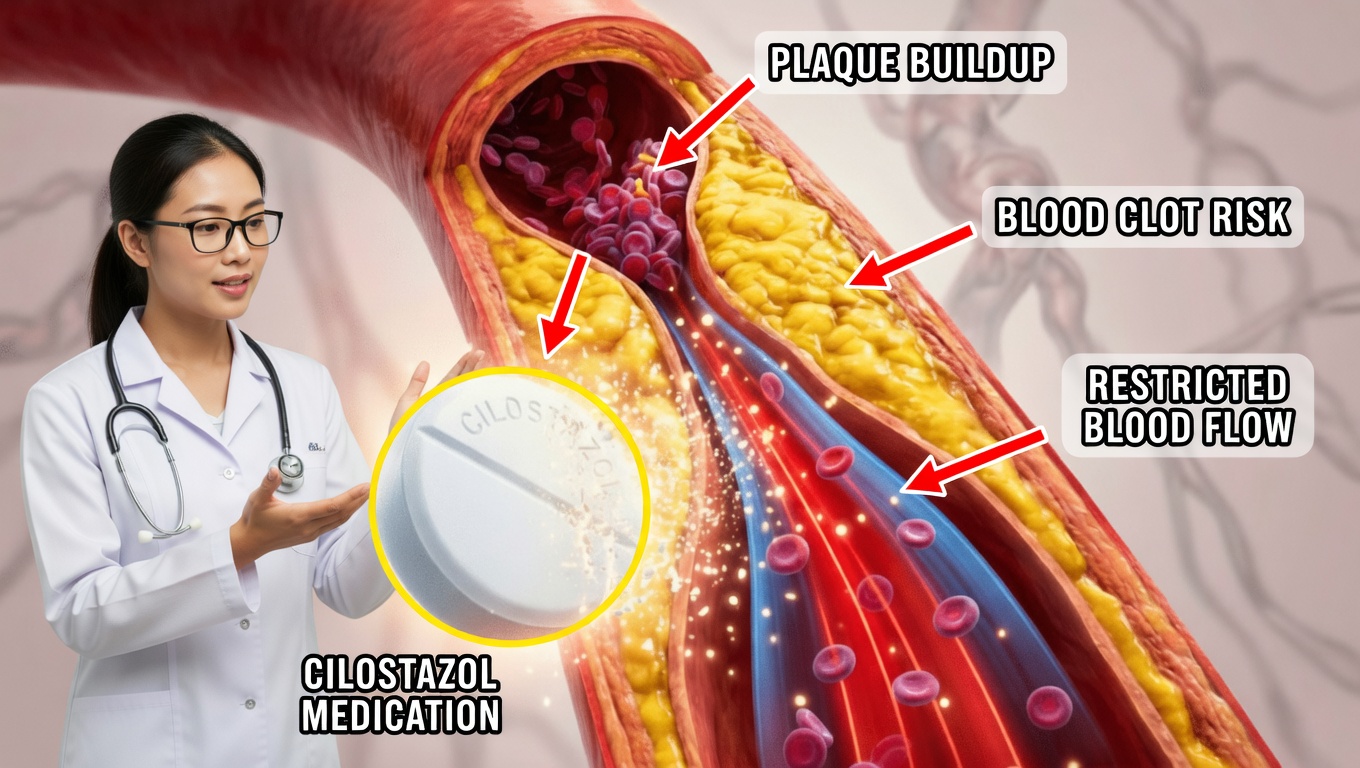
With atherosclerosis, a sticky substance called plaque builds up inside the artery walls. This plaque is made of:
- Fats
- Cholesterol
- Calcium
- Other blood components
Over years, this buildup hardens and narrows the arteries, restricting blood flow—similar to a water pipe slowly clogging with deposits. This process has been observed even in ancient Egyptian mummies, showing how long-standing and widespread the disease is.
When blood flow is reduced:
- Tissues receive less oxygen and nutrients
- Organs and muscles cannot function properly
- Serious conditions can develop, such as:
- Heart attacks (blocked arteries in the heart)
- Strokes (blocked arteries in the brain)
- Peripheral arterial disease (PAD) (blocked arteries in the arms or legs)
Cilostazol is mainly used to treat symptoms of PAD affecting the legs.
2. Intermittent Claudication: The Classic Symptom of Blocked Leg Arteries
When atherosclerosis affects the arteries in your legs, the condition is called Peripheral Arterial Disease (PAD). The hallmark symptom of PAD is intermittent claudication—a cramping or aching pain in your leg muscles (usually the calves, but sometimes the thighs or hips) that appears with activity and eases with rest.
Here’s what happens:
- When you walk or exercise, your leg muscles need more oxygen.
- Because the arteries are narrowed, they can’t deliver enough blood.
- The lack of oxygen causes pain, cramping, or fatigue in the muscles.
- When you stop walking, oxygen demand falls, and the pain improves.
- When you start again, the pain returns—creating a “walk–rest–walk” pattern.
As PAD gets worse:
- The distance you can walk before pain starts becomes shorter
- Daily activities like shopping or climbing stairs become difficult
- In advanced cases, you may experience:
- Pain even at rest (especially at night)
- Non-healing wounds or ulcers on the feet or legs
Cilostazol is prescribed to help reduce this pain and allow people with claudication to walk longer distances.
3. How Does Cilostazol Work?
Cilostazol belongs to a group of drugs known as phosphodiesterase 3 (PDE3) inhibitors. While the name is technical, its effects are relatively straightforward. The medicine improves circulation in two key ways:
3.1 Vasodilation: Widening the Arteries
Cilostazol relaxes the smooth muscle cells in the walls of your arteries. This relaxation causes the vessels to widen (dilate), especially in the legs.
- Wider arteries = more room for blood to flow
- More blood flow = better oxygen delivery to your muscles
You can think of it like opening up a narrowed pipe so more water can pass through.
3.2 Antiplatelet Effect: Making Blood Less “Sticky”
Cilostazol also has an antiplatelet effect:
- Platelets are small blood cells that help form clots.
- In atherosclerosis, platelets can stick to plaque and form clots that may completely block a narrowed artery.
- Cilostazol reduces the tendency of platelets to clump together, helping to maintain smoother blood flow through diseased arteries.
By combining vasodilation and antiplatelet activity, Cilostazol helps relieve the symptoms of intermittent claudication and can increase the distance you’re able to walk without pain.
4. Arteries vs. Veins: Why Cilostazol Is Not for Varicose Veins or DVT
One of the most important things to understand is that not all circulation problems are the same. Arterial disease and venous disease are different conditions, and they require different treatments.
- Arteries: Carry oxygenated blood away from the heart to the body.
- Veins: Carry deoxygenated blood back to the heart.
4.1 Arterial Disease: Where Cilostazol Works
Atherosclerosis is a disease of the arterial system. Plaque builds up inside the artery walls, narrowing them and restricting flow. Cilostazol acts on arteries, improving blood flow in people with PAD and intermittent claudication.
4.2 Venous Disease: Where Cilostazol Does Not Help
Venous conditions include:
- Varicose veins: Dilated, twisted veins caused by weakened vein walls and faulty valves. They are not blocked by plaque.
- Deep vein thrombosis (DVT): A blood clot forming in a deep vein, usually in the leg, often linked to prolonged immobility, surgery, or clotting disorders.
Cilostazol is not used to treat these venous problems.
- DVT is treated with anticoagulants (blood thinners) such as Warfarin, Rivaroxaban, Apixaban, or Heparin, which prevent clots from growing and reduce the risk of pieces breaking off and causing a pulmonary embolism.
- Varicose veins are managed with lifestyle measures, compression stockings, and sometimes procedures like sclerotherapy, laser treatment, or surgery.
Using Cilostazol for varicose veins or DVT would be inappropriate and ineffective. It is specifically indicated for arterial circulation issues, not vein disease.
5. Cilostazol as Part of a Comprehensive Treatment Plan
Cilostazol is not a cure for atherosclerosis or peripheral artery disease. It is a supportive medication that works best when combined with a broader treatment strategy.
5.1 Lifestyle Changes: The Foundation
No medication can fully overcome unhealthy habits. To slow or reverse the progression of atherosclerosis, you must tackle the root causes. Essential lifestyle changes include:
- Stopping smoking: Smoking is one of the strongest risk factors for PAD. Quitting is critical.
- Eating a heart-healthy diet: Focus on fruits, vegetables, whole grains, lean proteins, and healthy fats; limit saturated fats, trans fats, and processed foods.
- Regular physical activity: Supervised or structured walking programs are particularly effective for improving claudication symptoms.
- Managing blood pressure, cholesterol, and blood sugar: Proper control of hypertension, high cholesterol, and diabetes is crucial.
Without these changes, plaque will continue to build up and circulation will likely worsen, regardless of medication.
5.2 Other Key Medications
Cilostazol is often prescribed alongside two other major drug categories:
-
Antiplatelet agents
- Examples: Aspirin, Clopidogrel
- Purpose: Prevent platelets from forming clots on plaques; reduce risk of heart attack and stroke.
-
Statins (cholesterol-lowering medications)
- Examples: Atorvastatin, Rosuvastatin, Simvastatin
- Purpose: Lower LDL (“bad”) cholesterol and help stabilize existing plaque, making it less likely to rupture and cause a sudden blockage.
Together with lifestyle measures, these drugs target both the symptoms (e.g., leg pain when walking) and the underlying disease process.
5.3 Where Cilostazol Fits In
Cilostazol is mainly used to:
- Improve walking distance
- Reduce pain and cramping associated with intermittent claudication
- Enhance overall functional capacity and quality of life
However, taking Cilostazol while continuing to smoke heavily, eat poorly, and remain sedentary will greatly limit its benefits. It is most effective as part of a multifaceted PAD management plan.
6. Side Effects and Safety Considerations
Like all medications, Cilostazol can cause side effects and is not suitable for everyone. Because it improves blood flow throughout the body and affects blood vessels and heart function, careful medical supervision is essential.
6.1 Common Side Effects
Some of the more frequently reported side effects include:
- Headache
- Dizziness or lightheadedness
- Palpitations (feeling your heart beating fast or irregularly)
- Diarrhea or loose stools
- Stomach discomfort or abdominal pain
- Swelling (edema), especially in the ankles or legs
These symptoms are often mild and may improve over time, but any persistent or bothersome effect should be discussed with your doctor.
6.2 Who Needs to Be Especially Careful?
Cilostazol is not appropriate for certain patients, including many with specific heart conditions. In particular:
- It is generally contraindicated in people with heart failure, because drugs that act like Cilostazol (PDE3 inhibitors) have been associated with increased mortality in heart failure patients.
- People with serious heart rhythm problems, recent heart attacks, or uncontrolled high blood pressure may need alternative treatments.
- Those taking multiple medications must be monitored for drug interactions, especially with drugs that affect liver metabolism or other blood thinners.
Your healthcare provider will review your:
- Medical history
- Current medications
- Overall cardiovascular risk
before deciding whether Cilostazol is safe and appropriate for you.
6.3 The Importance of Medical Guidance
Because of its effects on blood flow and platelets, you should never start, stop, or change the dose of Cilostazol on your own. Always:
- Follow the prescribed dose and schedule
- Inform your doctor about any new symptoms (chest pain, shortness of breath, severe headache, sudden weakness, or signs of bleeding)
- Keep regular follow-up appointments to monitor your response and adjust treatment as needed
Final Thoughts
Cilostazol is a powerful and valuable medication for people with peripheral artery disease and intermittent claudication, helping them walk farther and live more independently. However, it:
- Works on arteries, not veins
- Does not replace lifestyle changes
- Must be used as part of a comprehensive treatment plan
- Requires careful medical supervision, especially in people with heart conditions
If you suspect you have poor circulation or PAD symptoms, consult a healthcare professional. They can determine whether Cilostazol has a role in your treatment and guide you toward the safest and most effective plan for protecting your circulation and overall cardiovascular health.