Constant Throat Mucus: What It Really Means and How to Fix It Naturally
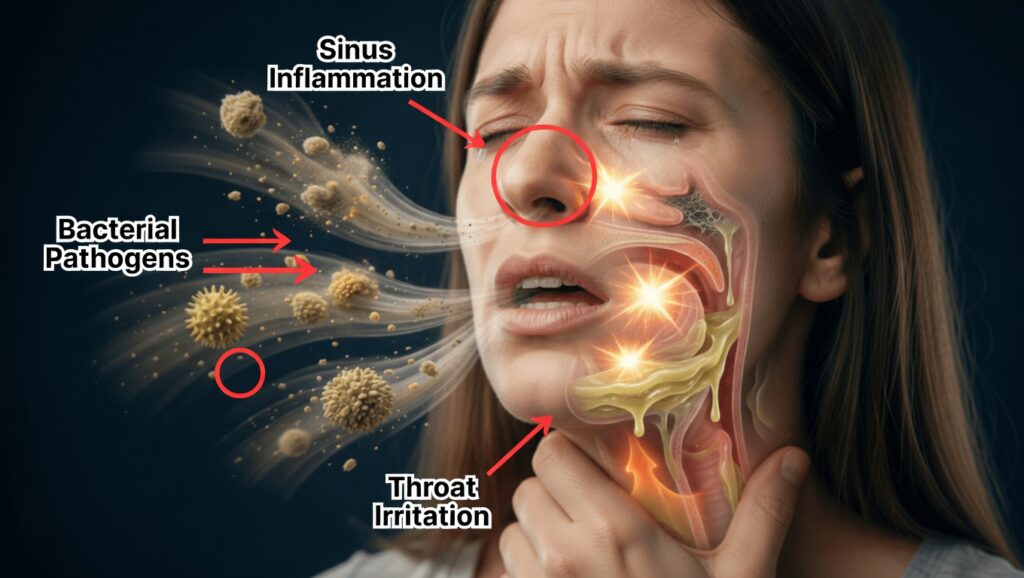
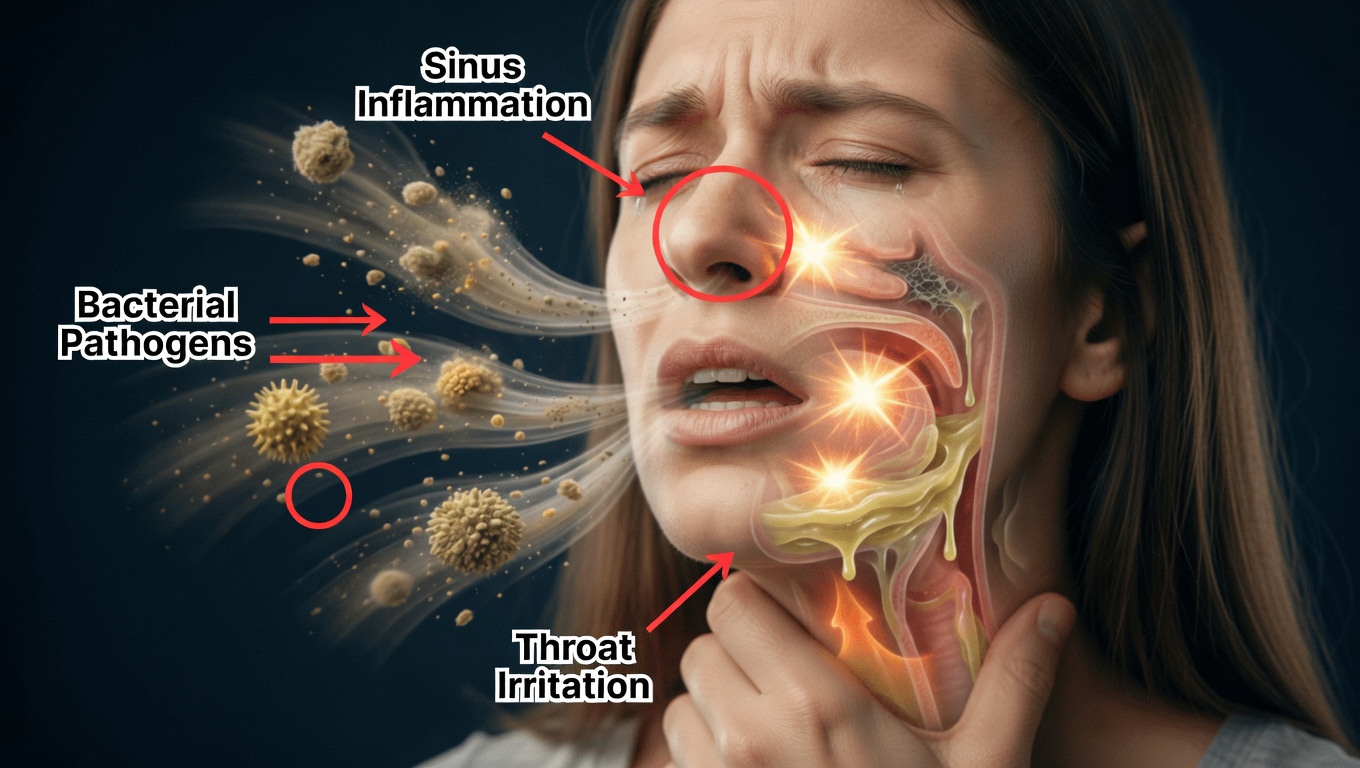
Do you constantly feel a lump or thick mucus at the back of your throat? Are you always clearing your throat, sometimes to the point of irritation or pain? You’re far from alone. Persistent throat mucus—often called post‑nasal drip—affects millions of people and can seriously disrupt sleep, speech, work, and daily comfort.
Most of us instinctively reach for quick‑fix medications to shut down the symptom. The issue? Many conventional treatments, including repeated courses of antibiotics, only offer short‑term relief. They may also trigger side effects, disrupt your gut and immune system, and even promote fungal overgrowth or antibiotic‑resistant bacteria.
In this guide, we’ll move beyond symptom control and look at what’s actually driving your excess mucus—and how to address it safely, naturally, and more permanently.
Important Note Before You Begin
This article is for informational and educational purposes only. It does not replace a medical consultation and cannot provide personalized medical advice. Always speak with your doctor or qualified health professional before changing any treatment, medication, or supplement.
(Insights adapted from the work of Sento Farmacéutico.)
Key Takeaways
-
Look Deeper Than the Mucus Itself
Chronic mucus is often a warning sign, not the core problem. Only suppressing it with drugs can miss the real cause and create new health issues. -
Four Common Root Causes
The most frequent and easily overlooked triggers include:- Gastroesophageal reflux (including “silent” reflux)
- Persistent sinus infections and biofilms
- Hypothyroidism (underactive thyroid)
- Hidden allergies or sensitivities
-
Reflux Isn’t Always “Too Much Acid”
For many people, reflux stems from low stomach acid, not excess. When stomach acid is insufficient, the valve between the esophagus and stomach may not close properly, allowing contents to flow upward. -
Natural Strategies Can Be Highly Effective
Tools such as saline nasal rinses, strategic dietary changes (for example, trial removal of dairy), targeted supplements, and intermittent fasting can help resolve underlying causes and give more lasting relief.
1. The Unexpected Trigger: Gastroesophageal Reflux (GERD)
One of the most common—and often surprising—drivers of chronic throat mucus is gastroesophageal reflux disease (GERD). Reflux occurs when stomach contents, including acid, travel up the esophagus and reach the throat and larynx.
This irritates the delicate tissues of your upper airway. In response, your body produces extra mucus as a protective barrier. The result can be:
- A constant feeling of mucus or a “lump” in the throat
- Frequent throat clearing
- Chronic cough or hoarseness
The standard treatment is typically proton pump inhibitors (PPIs) such as omeprazole, esomeprazole, or pantoprazole. Millions of people take these medications for months or even years.
However, long‑term use of PPIs has been linked with:
- Vitamin and mineral deficiencies (e.g., B12, magnesium)
- Increased risk of bone problems
- Disruption of the gut microbiome
- Rebound acid hypersecretion (worsened reflux) after stopping
When Reflux Comes from Too Little Acid
Contrary to popular belief, reflux isn’t always caused by excessive acid. In many people, it may be due to hypochlorhydria, or low stomach acid.
Here’s why that matters:
- The lower esophageal sphincter (LES)—the valve between the esophagus and stomach—needs a sufficiently acidic environment to close tightly.
- When stomach acid is too low, the LES may stay slightly open.
- This allows food and acid to splash back up, leading to reflux symptoms and throat irritation.
While hypochlorhydria is not widely recognized in conventional medicine and human studies are still limited, it is a physiologically plausible concept frequently used in functional and integrative medicine.
A Simple At‑Home Indicator (Not a Diagnosis)
A commonly used indicative self‑test (not a diagnostic tool) is:
- Dilute 1 tablespoon of apple cider vinegar in a glass of water.
- Drink it shortly before a main meal.
- Notice whether your reflux or throat symptoms improve, worsen, or stay the same.
If you feel better, it may suggest that your stomach acid was too low rather than too high. If it burns or worsens your symptoms, stop immediately and discuss with your doctor.
Betaine HCl: A Functional Medicine Tool
Another approach used in functional medicine is betaine hydrochloride (HCl), a supplement that provides hydrochloric acid to help acidify the stomach when taken with meals.
Important cautions:
- Do not use betaine HCl if you have:
- A known or suspected stomach or duodenal ulcer
- Active gastritis
- You are taking NSAIDs or other medications that irritate the stomach
- Always start only under medical supervision, as this is a potent intervention that can cause harm if misused.
2. The Hidden Residents: Chronic Sinus Infections and Biofilms
Another major source of ongoing mucus is chronic sinus infection. This is different from an acute sinus infection that clears after a week or two of antibiotics. Chronic sinusitis can drag on for months—or even years.
At the center of many persistent cases are biofilms.
What Are Biofilms?
Imagine a well‑protected “city” of bacteria, fungi, and other microbes attached to the lining of your sinuses. They encase themselves in a sticky, slimy matrix—a protective mucous shield that:
- Blocks antibiotics from reaching them effectively
- Shields them from your immune defenses
- Allows them to survive and continue causing inflammation
These entrenched communities:
- Keep producing inflammatory substances
- Stimulate continuous mucus production
- Lead to post‑nasal drip and constant throat clearing
You might feel better right after antibiotics, only for symptoms to return weeks later. Over time, repeated antibiotic use can encourage resistant strains that are even harder to treat.
Nasal Irrigation: A Simple Yet Powerful Tool
To tackle chronic sinus issues and biofilms, one of the most effective natural options is nasal irrigation with saline—often performed with a Neti pot.
A Neti pot is a small pot (similar to a tiny teapot) used to gently pour saltwater into one nostril so it flows out the other. It may sound strange, but it works through:
-
Mechanical Action
- The flow of saline physically flushes out:
- Thick mucus
- Allergens
- Microbial fragments and parts of biofilms
- The flow of saline physically flushes out:
-
Biological Stimulation
- Your nasal passages and sinuses are lined with tiny hair‑like structures called cilia.
- Their job is to move mucus outward.
- Inflammation and infection can paralyze or slow them.
- Saline solution helps reactivate and support their normal movement.
How to Use Nasal Irrigation Safely
- Use sterile, distilled, or previously boiled and cooled water mixed with salt.
- You can also use commercial isotonic saline or seawater solutions.
- Never use straight tap water without proper sterilization, as it may contain harmful microorganisms.
- For active or severe sinus inflammation, hypertonic saline (a slightly more concentrated salt solution) is sometimes used to reduce swelling—ideally under professional guidance.
If you’ve had stubborn throat mucus for months, a trial of daily nasal irrigation for about two weeks can often bring noticeable relief, sometimes within just a few days.
3. The Overlooked Link: Hypothyroidism (Low Thyroid Function)
A third, frequently missed cause of chronic mucus is hypothyroidism, or an underactive thyroid gland.
Your thyroid produces hormones that control the speed of your metabolism—essentially the “pace” at which your body works. When thyroid function is low, everything slows down, including the mechanisms that keep mucus flowing and draining properly.
How Hypothyroidism Promotes Mucus Buildup
- The cilia in your nose, sinuses, and throat depend on adequate thyroid hormone to move efficiently.
- With hypothyroidism, these cilia can become sluggish.
- Mucus doesn’t get cleared as it should, so it accumulates and thickens.
- This can lead to that familiar feeling of sticky mucus in the throat, often worse in the morning.
Signs Your Thyroid Might Be Involved
If you have chronic mucus along with some of these symptoms, hypothyroidism is worth investigating:
- Persistent fatigue or low energy
- Unexplained weight gain or difficulty losing weight
- Dry skin and hair
- Sensitivity to cold
- Constipation
- Thick, hard‑to‑clear mucus in the throat
If this sounds like you, ask your doctor for a comprehensive thyroid panel, not just a TSH. This may include free T4, free T3, thyroid antibodies, and other markers to get a fuller picture of thyroid function.
4. The Immune Overreaction: Allergies and Sensitivities
Finally, a very common driver of ongoing mucus is allergy—your immune system overreacting to substances that are normally harmless.
When your body perceives an allergen as a threat, it releases chemicals like histamine. This leads to:
- Inflammation of the nasal and throat tissues
- Swelling
- Increased mucus production
Environmental Allergies
Common environmental triggers include:
- Pollen (grass, trees, weeds)
- Dust mites
- Molds
- Pet dander
These allergies may flare up in certain seasons or be present all year, depending on your environment.
If you suspect environmental allergies:
- An allergist can perform skin prick tests or specific blood tests to identify what you react to.
- Reducing exposure, using air purifiers, and following a tailored treatment plan can significantly cut down mucus production.
Food-Related Reactions: The Dairy Debate
Food allergies and sensitivities can also contribute to mucus in some individuals. Among these, dairy products (milk, cheese, yogurt, cream) are often discussed in relation to throat mucus and post‑nasal drip.
The science here is nuanced:
- The most rigorous studies generally do not consistently show that dairy increases mucus production in the general population.
- However, some people report noticeably thicker mucus, congestion, or throat discomfort when they consume dairy—and improvement when they avoid it.
Because individual responses vary, a practical approach is:
- Try a short‑term elimination of dairy (for example, 2–4 weeks).
- Track changes in your mucus, congestion, or throat symptoms.
- Reintroduce dairy and see if symptoms return or worsen.
If you notice a clear pattern, discuss it with your doctor or nutrition professional to ensure your diet remains balanced while avoiding problematic foods.
By understanding the deeper causes of chronic mucus—reflux, sinus biofilms, thyroid function, and allergies—you can move beyond temporary symptom relief and work toward real, lasting change. Always partner with a healthcare professional to evaluate your specific situation and design a safe, personalized plan.