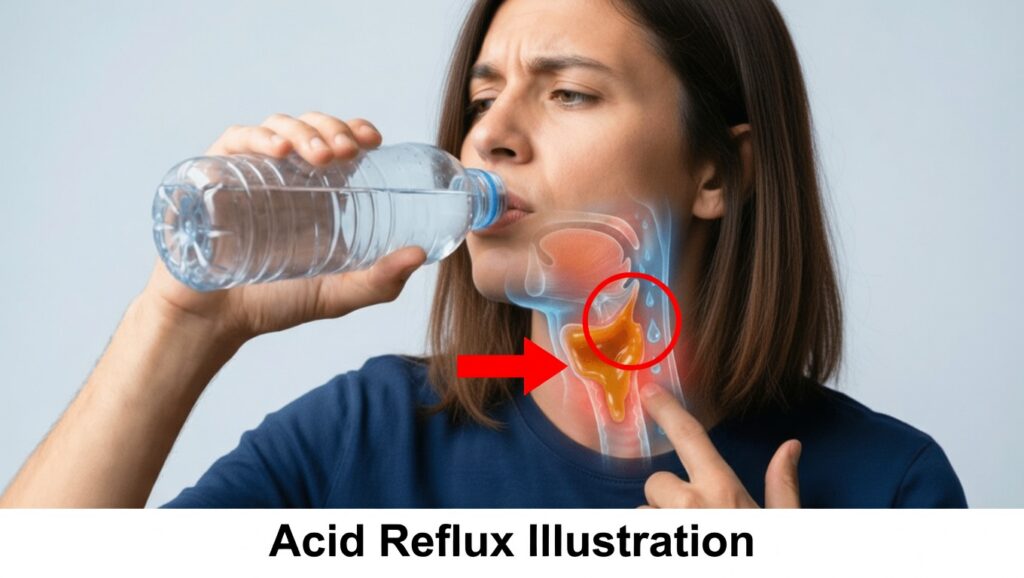
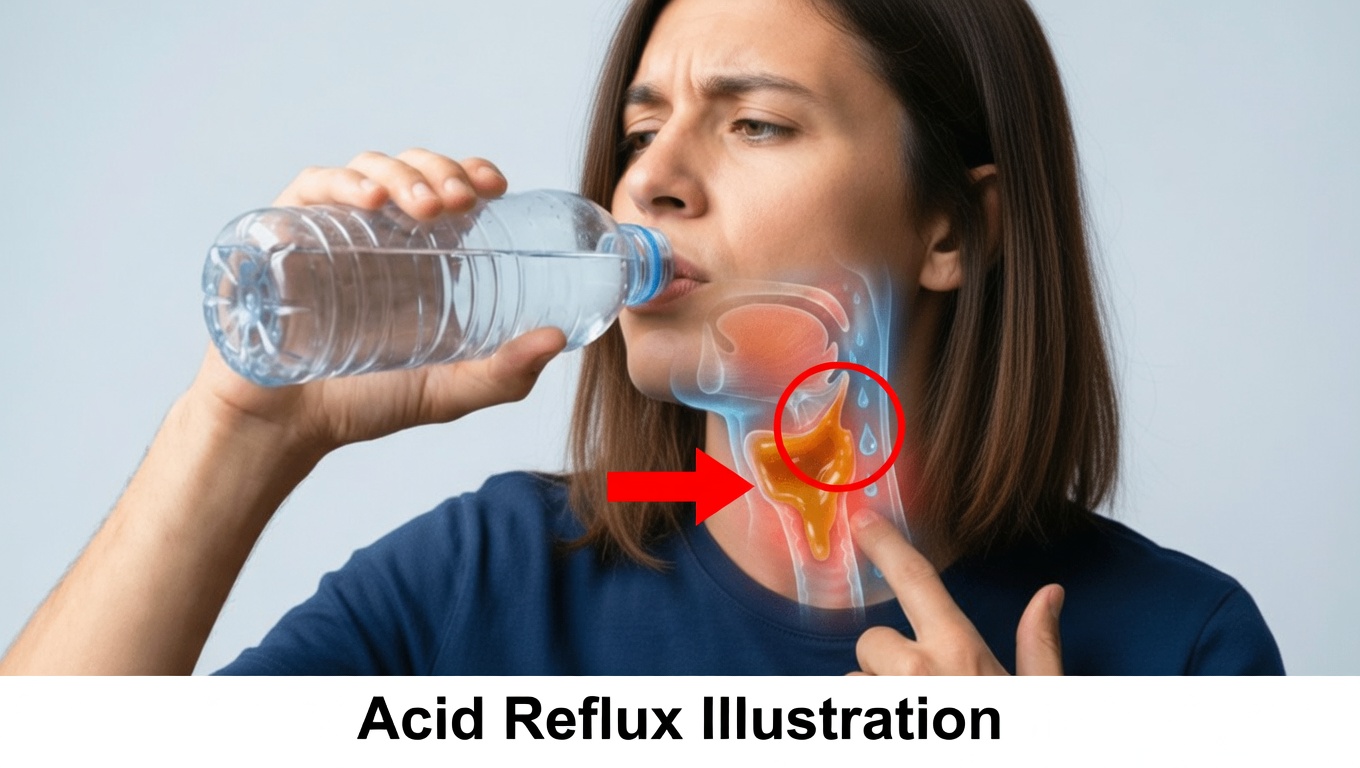
Why It Feels Like Something Is Stuck in Your Throat (and Why Water Isn’t Helping)
If you live with a constant urge to clear your throat, feel “phlegm” that never quite goes away, or have a stubborn lump sensation that doesn’t move no matter how often you swallow, you’re not imagining it.
You may have tried the usual advice: drink more water, sip herbal tea, stay hydrated. Yet the feeling remains. For some people, it even seems worse after doing all that. So what’s really going on?
In many cases, the problem isn’t simple mucus or dryness—it’s a digestive enzyme that has climbed out of your stomach and taken up residence in your throat. And this “chemical squatter” doesn’t respond to plain water any more than engine grease does.
The explanation below is based on the work of physicians such as Dr. Alberto Sanagustín and research on silent reflux and pepsin.
Key Takeaways
- That persistent lump or “phlegm” in your throat (often called globus sensation) is frequently not just mucus; it is often linked to pepsin, a digestive enzyme that has refluxed up from your stomach.
- Pepsin can rise into the throat as a gas or fine mist in a process known as silent reflux, then bind to the lining of your throat and voice box.
- Plain water doesn’t remove it because pepsin is hydrophobic—it repels water, similar to how oil or grease resists water.
- When you consume acidic foods and drinks (such as citrus, tomatoes, coffee, soda, or certain sauces), they can reactivate this pepsin in your throat, causing irritation, inflammation, and extra mucus production.
- A practical three-step strategy can help:
- Neutralize pepsin with alkaline gargles
- Limit new reflux with alginate “raft” products
- Avoid acidic triggers temporarily to stop reactivating the enzyme
- Urgent warning: If you have trouble swallowing, swallowing pain, unexplained weight loss, blood in saliva or phlegm, a new neck lump, or voice changes lasting more than a few weeks, you must seek immediate medical assessment.
1. Why Your Water Bottle Isn’t Fixing That Lump in Your Throat
Staying hydrated is essential for health, but when it comes to that specific stuck or phlegmy feeling in your throat, endlessly sipping water often does almost nothing.
Think of it like trying to wash thick engine grease off your hands using only cold tap water. The water just slides over the greasy layer. It doesn’t dissolve or remove it, because grease and water don’t mix. You need soap—something with the right chemistry to break the grease down.
The substance causing your throat symptoms behaves in a similar way. The main suspect is a sticky protein enzyme that:
- Clings to the tissue in your throat
- Is hydrophobic (water-repelling), so water doesn’t dissolve or dislodge it
- Remains stuck even though you keep drinking
So you can drink liters of water, feel well-hydrated, and still feel that “glob” in your throat. The issue isn’t that you’re not drinking enough; it’s that the chemical nature of what’s sitting there is resistant to water.
In other words, you don’t just have a dryness problem—you likely have a biochemical problem that plain water can’t fix.
2. Meet the Real Culprit: Pepsin, the Chemical Squatter in Your Throat
So what is this water-resistant substance?
In many people, the main culprit is pepsin, a powerful digestive enzyme. Under normal conditions, pepsin:
- Lives in your stomach
- Helps break down dietary proteins (from meat, fish, eggs, dairy, etc.)
- Works best in a highly acidic environment
Inside the stomach, pepsin is doing exactly what it’s supposed to do. The problem starts when material from your stomach manages to move upward.
Most people know about acidic reflux that causes classic heartburn—the burning sensation in your chest when acid splashes up the esophagus. Pepsin, however, can travel differently:
- It can rise as a gas or aerosol—a very fine, invisible mist
- This mist can reach higher up, all the way to the throat and voice box
- Once there, pepsin can settle on and bind to the lining of your pharynx and larynx
This process is often called silent reflux or laryngopharyngeal reflux (LPR) because you may not feel typical heartburn. Instead, you get throat symptoms: a lump sensation, chronic throat clearing, hoarseness, or extra mucus.
Here’s the crucial part: once pepsin sticks to your throat tissues, it can lie dormant—inactive and waiting. You may not feel much when it first arrives. The trouble starts when something wakes it up.
3. Reactivation: How Your Food “Turns On” Pepsin in Your Throat
Pepsin is designed to function in an acidic environment. That’s why it’s so effective in the stomach.
When pepsin is stuck to your throat and you consume something acidic, you provide exactly what it needs to switch back on. Common triggers include:
- Citrus fruits (oranges, lemons, grapefruit, lime)
- Tomatoes and tomato-based products (sauces, ketchup, pizza, pasta sauces)
- Soft drinks and energy drinks
- Vinegar-based dressings or pickles
- Coffee and many teas
- Chocolate
- Alcohol (especially wine, beer, and spirits)
- Spicy or heavily seasoned foods
When these acidic foods or drinks come into contact with pepsin on your throat lining:
- The acid reactivates pepsin.
- The enzyme resumes its normal job—digesting proteins.
- But now, instead of breaking down food, it starts breaking down the protein in your own throat tissue.
This leads to:
- Irritation and inflammation of the throat lining
- A raw, scratchy, or burning feeling
- A constant need to clear your throat
- A sensation of thick mucus or a lump that doesn’t go away
The “phlegm” you notice is often your body’s defense mechanism: your throat produces extra mucus to protect itself from this chemical attack. Unfortunately, the extra mucus itself is uncomfortable and leads to more throat-clearing, which further irritates the tissue—a vicious cycle.
4. A 3-Step Protocol to Remove the Chemical Squatter
Before trying any home strategies, there is a crucial safety warning.
Important: Red-Flag Symptoms
Do not rely on home remedies alone if you notice any of the following:
- Difficulty swallowing food or liquids
- Pain when swallowing
- Unexplained weight loss
- Blood in saliva, phlegm, or from the mouth
- A new or growing lump in the neck
- Persistent hoarseness or voice change lasting more than 3–4 weeks
- Ongoing cough or throat symptoms in someone with a history of heavy smoking or alcohol use
These can be signs of more serious conditions and must be evaluated urgently by a doctor or ENT specialist.
If you do not have these warning signs and your doctor has not found a serious cause, you can consider the following three-step approach, ideally after discussing it with a healthcare professional.
Step 1: Neutralize Pepsin – Your “Chemical Soap”
Since plain water doesn’t inactivate pepsin, the goal is to change the pH around it. Research suggests that pepsin becomes permanently inactive at a pH above about 8 (alkaline).
A simple way to create an alkaline environment in your throat is with alkaline gargles.
Option A: Baking Soda Gargle
- Mix 1 teaspoon of baking soda (sodium bicarbonate) in a glass of water.
- Gargle deeply for about 30 seconds, making sure the mixture reaches the back of your throat.
- Spit it out. Do not swallow the solution.
- Repeat after meals and before bed, unless advised otherwise by your doctor.
Option B: Alkaline Water Gargle
- Use bottled alkaline water labeled with a pH of 8 or higher.
- Gargle as above and spit it out.
By raising the pH in the throat, you are essentially switching off pepsin that has settled on the tissues. Many people notice a reduction in throat irritation and mucus within 24–48 hours of consistent use.
Caution:
If you have kidney disease, heart failure, uncontrolled high blood pressure, are on a low-sodium diet, or take multiple medications, speak to your doctor or pharmacist before using baking soda regularly.
Step 2: Build a Barrier – Using Alginate “Rafts”
Neutralizing the enzyme in your throat is only half the battle. You also want to stop more pepsin from coming up.
This is where alginate-based products come in. Over-the-counter formulas containing sodium alginate (such as Gaviscon Advance in the UK/Canada and similar products elsewhere) can help by forming a physical barrier.
How they work:
- When taken after a meal, alginate reacts with stomach contents to form a gel-like “raft”.
- This raft floats on top of the stomach contents like a lid.
- It helps prevent both liquid acid and pepsin-rich aerosol from refluxing up into the esophagus and throat.
How to use them effectively:
- Take the alginate product right after you finish eating (follow the specific instructions on the label).
- Avoid drinking a large amount of fluid immediately afterward, as this can dilute or break up the raft.
- A small sip of water is usually fine, but skip the big post-meal drinks if possible.
This step doesn’t directly remove pepsin from your throat, but it reduces new exposure, giving your tissues a chance to calm down and heal.
Step 3: Stop Waking the Beast – Short-Term Elimination of Triggers
Even if you neutralize existing pepsin and block new reflux, you can still run into trouble if you keep reactivating what’s already there with acidic foods and drinks.
For 2–3 weeks, try a structured elimination of the most common triggers. During this time, reduce or avoid:
- Citrus fruits: oranges, mandarins, grapefruit, lemons, limes, and their juices
- Tomatoes: fresh tomatoes, tomato sauces, ketchup, pizza and pasta sauces
- Carbonated drinks: soda, sparkling water, energy drinks
- Coffee and caffeinated teas (including green tea, in some people)
- Chocolate (especially dark or very rich chocolate)
- Alcohol: wine, beer, and spirits
- Spicy foods: chili, hot sauces, heavily spiced meals
- Vinegar-heavy foods: pickles, some salad dressings, certain condiments
- Very greasy or fried foods, which can worsen reflux in general
- Large, late-night meals close to bedtime
During this trial period:
- Focus on low-acid, simple foods (e.g., oats, bananas, non-citrus fruits, steamed vegetables, lean proteins, non-tomato sauces).
- Notice whether your throat clearing, lump sensation, or phlegm improves.
- After 2–3 weeks, you can gradually reintroduce foods one at a time to identify your personal triggers.
Combining this food strategy with alkaline gargles and alginates can be particularly effective for many people with silent reflux–related throat symptoms.
When to Get Checked: Don’t Ignore Serious Symptoms
While silent reflux and pepsin are common causes of chronic throat sensations, they are not the only possibilities. It’s important not to self-diagnose if your symptoms are concerning.
Seek prompt medical advice—ideally from your primary care doctor or an ENT specialist—if you notice:
- Trouble swallowing solid foods or liquids
- Pain in the throat or chest when you swallow
- Unintentional weight loss
- Blood in your saliva, phlegm, or from the mouth
- A new lump or swelling in the neck
- Hoarseness, a persistent change in your voice, or chronic cough lasting more than 3–4 weeks
- Worsening symptoms if you have risk factors like heavy smoking or alcohol use
A proper examination may include throat visualization, endoscopy, or other tests to rule out more serious conditions.
Final Thoughts
If you’ve been told to “just drink more water” for that stubborn lump or phlegm in your throat and it hasn’t helped, there’s a good reason. In many cases, the problem isn’t dryness or simple mucus; it’s pepsin from silent reflux sitting on your throat tissues, where water alone can’t touch it.
By:
- Neutralizing the enzyme with alkaline gargles,
- Blocking new reflux with alginate products,
- And avoiding acidic triggers that reactivate pepsin,
you may be able to break the cycle of irritation, inflammation, and excess mucus.
Always keep the warning signs in mind and seek medical evaluation if anything feels off. But if serious causes have been ruled out, understanding the role of pepsin and silent reflux can finally make sense of your symptoms—and give you practical tools to start feeling relief.