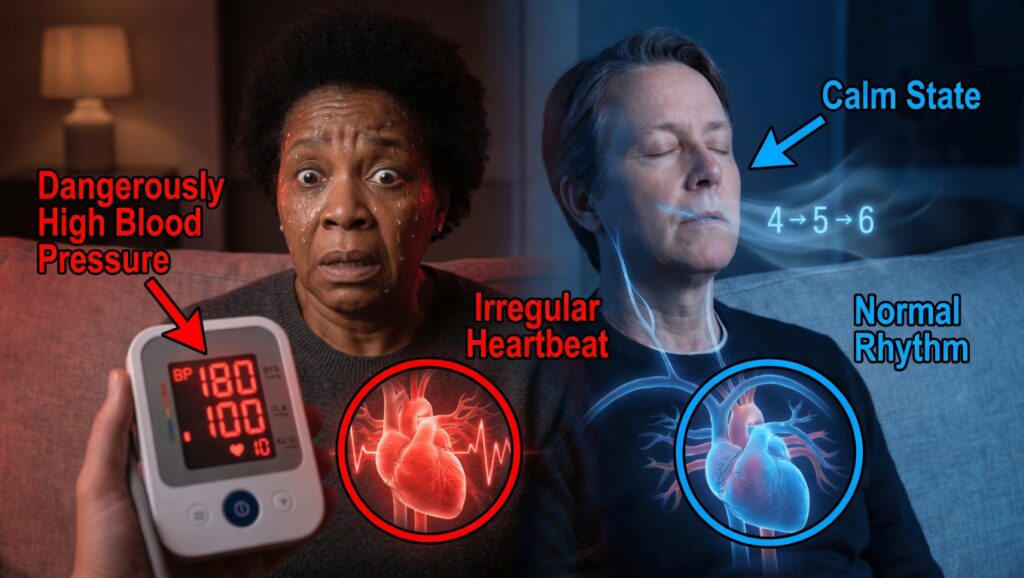
Blood Pressure 180/100 at Home: What It Really Means and What to Do
You’re at home, you put on your blood pressure cuff, and the screen shows 180 over 100. Your heart starts pounding, your mind races:
“Is this a heart attack? Am I having a stroke? Do I need to go to the emergency room right now?”
Before you rush out the door, pause. Understanding what those numbers actually represent—and how to respond calmly—can protect your health and prevent unnecessary panic.
This guide, inspired by the insights of cardiologist Dr. Juan Veller, explains:
- When a high blood pressure reading is serious
- What you can safely do at home to bring your numbers down
- Which “emergency” pills you should avoid
- How to recognize the warning signs that mean you must go to the ER
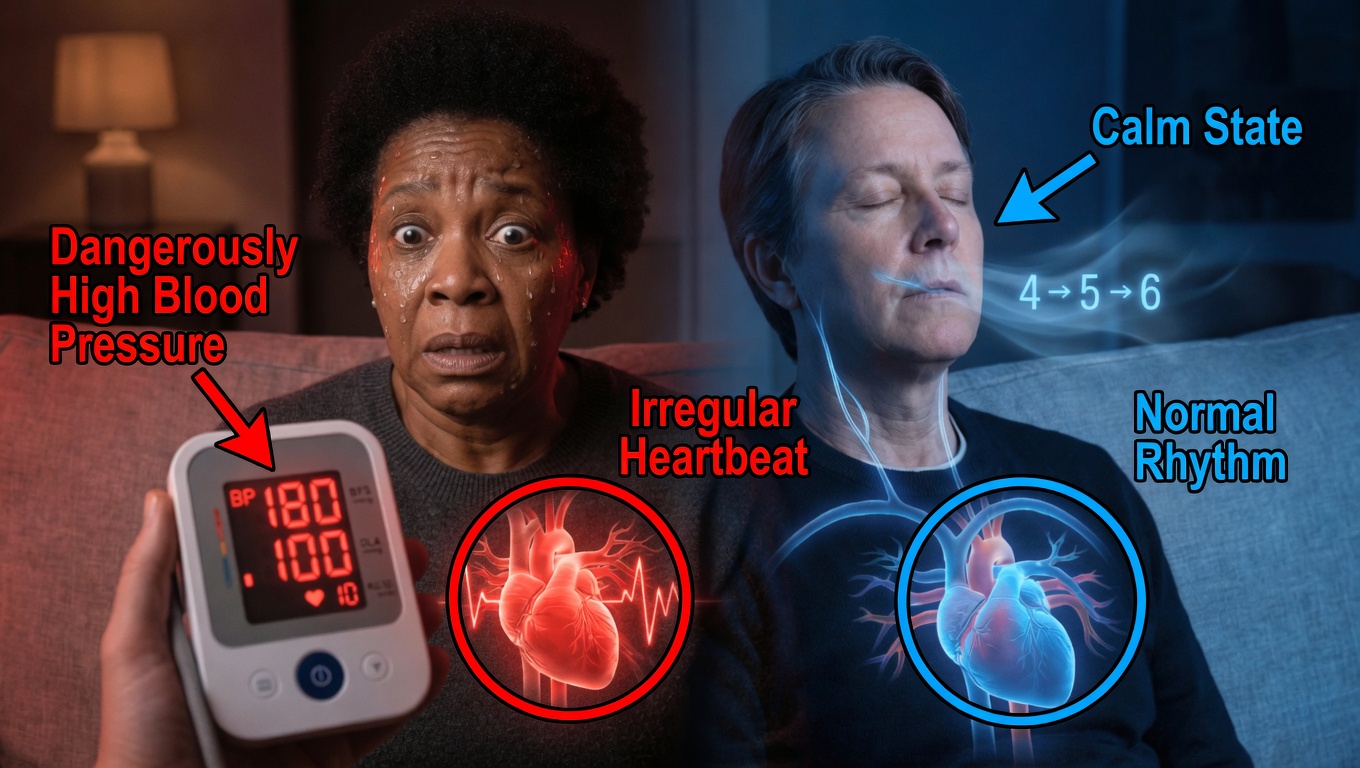
Key Takeaways
- A single high blood pressure reading at home (even 180/100) is rarely an emergency if you have no concerning symptoms.
- Taking extra medication or using fast-acting pills without medical guidance can be dangerous.
- Simple, evidence-based techniques can help calm your body and gently lower your blood pressure.
- Knowing the red-flag symptoms of a true emergency is essential so you can act fast when it really matters.
1. Don’t Panic: A High Number Alone Is Not Always an Emergency
Seeing 180/100 or similar numbers on your home blood pressure monitor is alarming, but it does not automatically mean you are in immediate danger.
Modern cardiology emphasizes this key idea: doctors treat people, not just numbers.
If you feel generally well and have no severe symptoms, a single elevated reading is usually not a medical emergency. Often, it reflects temporary stress, anxiety, or recent activity rather than a life-threatening crisis.
Take a slow breath and remind yourself: one high reading does not equal a stroke or heart attack.
2. Ask Yourself Two Essential Questions
Before you decide what to do next, check how you feel by asking:
-
Do I have any pain?
- Headache
- Chest pain
- Back pain (especially in the upper back)
-
Did something emotionally intense happen in the last few hours?
- An argument or conflict
- A stressful event at work or home
- Excitement, celebration, or shock
Emotional stress and strong feelings can cause temporary spikes in blood pressure. If you’re only experiencing mild discomfort (such as a light headache) and no other symptoms, most experts agree you usually do not need to rush to the emergency room.
3. Avoid Self-Medicating with Fast-Acting “Emergency” Pills
Friends, family, or the internet may suggest:
- Taking a pill under the tongue (sublingual medication)
- Doubling your usual blood pressure dose
- Using medication that was not prescribed for you
This is outdated advice and can be risky.
When your body has adapted to higher blood pressure, suddenly dropping it too fast can reduce blood flow to your brain, heart, and other organs, causing dizziness, fainting, and in severe cases, serious complications. Any change in medication—especially rapid, strong drops in blood pressure—should be supervised by a doctor.
Stick to your prescribed treatment and avoid “quick fix” pills unless your own physician has explicitly instructed you to use them in this way.
4. Break the Anxiety Loop: Don’t Check Your Blood Pressure Every Few Minutes
A common cycle looks like this:
- You see a high reading.
- You become more anxious.
- You recheck your blood pressure right away.
- The number is still high—or higher—so you get even more stressed.
This “BP-checking loop” keeps your nervous system on high alert and can keep your blood pressure elevated.
Instead, after a high reading:
- Use calming techniques first.
- Wait at least 20–30 minutes before checking again.
- Limit how often you measure your blood pressure during a stressful episode.
5. Proven Ways to Calm Down and Gently Lower Your Blood Pressure
When your blood pressure is high but you have no alarming symptoms, your first goal is to relax your body and mind. These strategies can help.
A. Real, Distraction-Free Rest
Give your nervous system a break:
- Turn off the TV, loud music, and put your phone aside.
- Dim the lights or move to a quieter room.
- Lie down or sit comfortably in a chair.
- Read something light or calming (avoid intense news or work emails).
- Avoid arguments, stressful conversations, and anything emotionally charged.
Even 15–20 minutes of real rest can make a noticeable difference in blood pressure.
B. Simple Pain Relief (If Needed)
If your blood pressure is up and you have a mild headache or backache:
- You can take a standard dose of a common over-the-counter pain reliever like acetaminophen (paracetamol), as long as it is safe for you and you have no contraindications.
- Drink a glass of water, especially if you might be dehydrated.
Relieving minor pain and correcting mild dehydration can reduce physical stress on your body. Do not exceed recommended doses and do not overuse pain medication.
C. The 4–5–6 Breathing Technique
Slow breathing is a powerful tool to activate your parasympathetic nervous system—the body’s natural “brake” that helps lower heart rate and reduce blood pressure.
Try this pattern:
- Inhale gently through your nose for 4 seconds.
- Hold your breath for 5 seconds.
- Exhale slowly through your mouth for 6 seconds.
- Repeat for 2–3 minutes in a quiet, comfortable place.
Focus on counting and on the air moving in and out. This simple technique can calm your nervous system and support a gentle drop in blood pressure.
6. When High Blood Pressure IS an Emergency: Red Flag Symptoms
A high reading like 180/100 becomes dangerous when it’s accompanied by signs that your heart, brain, or other organs may be in trouble. In these situations, you must seek emergency care immediately.
Go to the ER or call emergency services right away if high blood pressure comes with:
- Chest pain
- Pressure, tightness, burning, or heavy discomfort in the chest
- Different from typical indigestion or heartburn
- Shortness of breath
- Rapid breathing
- Feeling like you can’t get enough air
- Difficulty speaking in full sentences
- Neurological symptoms (possible stroke warning signs)
- Slurred or unclear speech
- Drooping on one side of the face
- Sudden weakness or numbness in an arm or leg
- Sudden blurred vision or loss of vision
- Confusion, trouble understanding, or difficulty walking
- The worst headache of your life
- Sudden, severe headache unlike your usual ones
- Pain you’d describe as “unbearable” or “explosive”
These symptoms may indicate a stroke, heart attack, or another hypertensive emergency. Do not wait to “see if it goes away.” Get medical help immediately.
7. Be Strategic: Monitor Your Blood Pressure and Follow Up with Your Doctor
If:
- You have a high reading at home
- You feel generally okay
- And the spike seems related to emotional stress or a specific event
…then use the calming techniques above and allow some time for your body to settle.
After that:
-
Start a simple blood pressure log
- Measure your blood pressure once in the morning, and optionally once in the evening, for a couple of weeks.
- Write down the date, time, reading, and how you felt.
-
Share this log with your doctor
- Even if your appointment is a week or two away, this information will help your doctor see patterns, adjust your treatment if needed, and make better decisions.
If you’re already on medication for high blood pressure:
- Take it exactly as prescribed—do not adjust doses on your own.
- Reduce salt and processed foods in your diet.
- Stay active with regular, moderate exercise (as approved by your healthcare provider).
- Avoid obsessing over every single reading—blood pressure naturally fluctuates throughout the day.
8. The Bottom Line: Stay Calm, Be Informed, and Act When It Truly Matters
Keep these principles in mind:
- One high reading rarely equals an emergency. Your overall condition and symptoms matter more than the number alone.
- Cardiologists focus on people, not just blood pressure values. Signs of organ damage or distress are what turn a spike into an emergency.
- Staying organized and calm helps far more than panic. Thoughtful monitoring, relaxation techniques, and proper follow-up with your doctor are your best tools.
Feeling scared when you see a high number is completely normal. But with the right knowledge, you can respond with confidence instead of fear.
If your blood pressure spikes again, remember this guide:
pause, check for symptoms, calm your body, and seek urgent care only if you notice the red-flag signs.
For anything uncertain or persistent, consult your doctor. Your health is a long-term journey—and you’re not alone in it.
Source: Based on the insights of cardiologist Dr. Juan Veller.