The Hidden Risk of Overtreatment After 65
Are you—or someone you care about—over the age of 65? If so, there’s an important medical trend you need to know about. A growing number of older adults are being overtreated, especially for high blood pressure, high cholesterol, and chronic pain. This pattern is quietly causing serious complications for millions of seniors.
Most physicians genuinely want to help their patients. The issue isn’t usually the individual doctor; it’s the healthcare system they operate in. Modern medicine often follows a “pill for every ill” mindset, pushing more drugs, higher doses, and increasingly aggressive targets—sometimes without enough consideration for age, frailty, or common sense.

It’s time to pause and ask: “Is all this treatment actually helping—or could it be hurting?”
Based on the insights of Dr. Suneel Dhand, this article explains three common areas where overtreatment is widespread and shows you how to have more balanced, informed discussions with your healthcare provider.
Key Takeaways
-
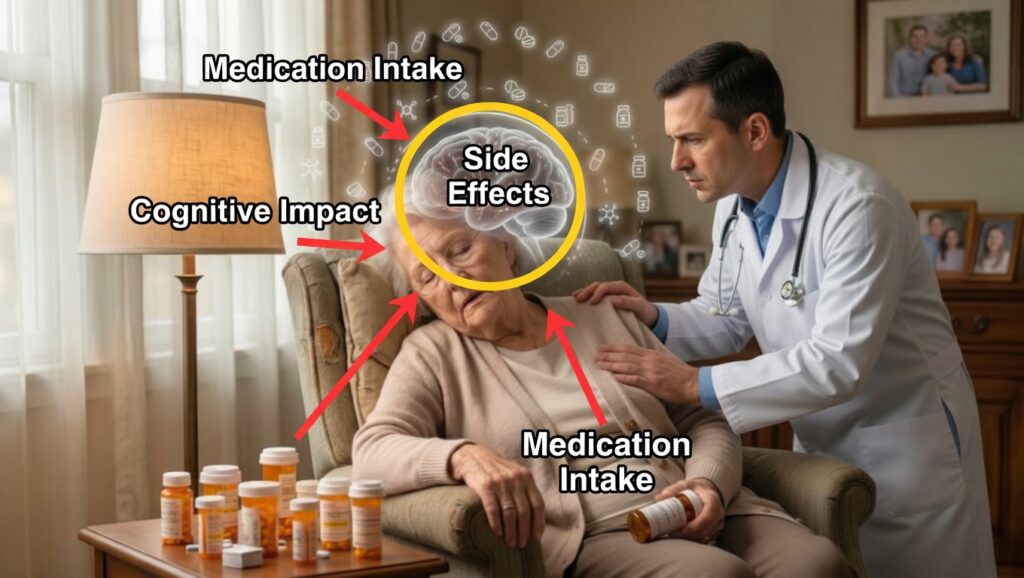
Overtreatment in Seniors: Many people over 65 are receiving more medication than they truly need—especially for blood pressure, cholesterol, and chronic pain—which can lead to dangerous side effects and reduced quality of life.
-
Blood Pressure in Older Adults: For seniors, pushing blood pressure too low can cause dizziness, falls, and possibly worsen thinking and memory. Regular home monitoring is essential to spot potential overmedication.
-
Cholesterol and Statins in the Elderly: Aggressively lowering cholesterol with high-dose statins in very old adults is not always supported by strong evidence for that age group and may negatively affect brain health.
-
Pain Medication Overload: Potent painkillers are often prescribed too quickly and at high doses, sedating older adults, increasing confusion, and fostering dependency—while safer, non-drug strategies are underused.
-
Your Role in Your Care: You need to be an active partner in your medical decisions—asking questions, understanding risk versus benefit, and exploring whether some medications can be reduced or stopped (“deprescribing”) under medical supervision.
1. High Blood Pressure: When “Lower” Isn’t Always Better in Older Age
Here’s a familiar pattern: someone starts a blood pressure medication in their 40s or 50s. Over time, one drug becomes two, then three. Those same prescriptions are carried into their 70s or 80s with little re-evaluation. What’s often overlooked is that the body changes dramatically with age.
As people get older, the arteries supplying the heart and brain tend to stiffen and calcify. Imagine a soft garden hose slowly turning into a rigid pipe. To keep blood flowing through this stiffer system—and to ensure the brain receives enough oxygen—your body may naturally require a slightly higher blood pressure. This concept is related to maintaining adequate cerebral perfusion pressure (the pressure needed to feed the brain with blood).
If a senior is taking multiple blood pressure medications aimed at hitting a younger person’s “perfect” numbers, that combination can push the blood pressure too low. When this happens, the consequences can be serious:
- Feeling lightheaded, weak, or unsteady
- A much higher risk of falls, which can be catastrophic in older adults
- Reduced blood flow to the brain over time, potentially contributing to cognitive decline and other neurological problems
These are not rare scenarios—they’re seen frequently in clinical practice.
So what can you do?
- If you or a loved one over 65 is on several blood pressure medications and experiences dizziness, fatigue, or frequent unsteadiness, start measuring blood pressure at home.
- Check at least three times a day for about two weeks to get a clear pattern.
- Pay particular attention to the systolic number (the top number). If it’s often in the low 100s (for example, 102, 104) or frequently dips into the 90s, this may indicate over-treatment.

Bring this data to your healthcare provider and ask whether your current targets are appropriate for your age and overall health. In some cases, it may be safer to carefully reduce or adjust medications rather than chase lower and lower numbers.
2. The Cholesterol Conundrum: Are We Chasing Numbers at Any Cost?
Over recent decades, medicine has launched an all-out war on cholesterol—especially LDL, the so‑called “bad” cholesterol. Guidelines have steadily tightened, pushing for LDL levels below 100 for many people, and under 70 for those with certain health conditions. This has led to widespread, high-dose statin use, even in very elderly patients.
A common situation looks like this: someone in their 80s is admitted to the hospital with chest pain or a possible stroke. They leave with a prescription for a high-dose statin, regardless of whether strong evidence exists for that age group.
Here’s the problem: many of the original clinical trials for statins did not include very old adults. We often take data from 55-year-olds and apply it directly to 85-year-olds, despite major differences in metabolism, muscle mass, brain function, and overall resilience.
It’s also important to remember what cholesterol actually does. Cholesterol is not a toxic invader; it is:
- A key component of every cell membrane
- Essential for hormone production
- Crucial for brain structure and function—your brain is roughly 60% fat and heavily depends on cholesterol
When cholesterol is aggressively driven down to very low levels, we must ask: what happens to the brain and other organs that rely on it? Reports of memory problems or cognitive changes have raised understandable concern.
This doesn’t mean everyone should abandon statins. But it does mean you should ask targeted, age-specific questions, such as:
- “For someone my age with my health history, what is the number needed to treat (NNT) for this statin?”
The “number needed to treat” tells you how many people must take a drug for one person to benefit. In many chronic disease medications, including some statins, this can be surprisingly low—sometimes 1 in 50 or even less favorable.
Then ask yourself:
- Am I comfortable taking on the potential side effects—muscle pain, fatigue, possible cognitive effects—for a 1 in 50 chance of benefit?
- Is our focus on improving a lab number, or on actually living longer and better?
It’s not about rejecting treatment; it’s about making sure that treatment is truly meaningful for your age, goals, and quality of life.
3. Aches and Pains: The Rush to Prescribe Powerful Pain Medications
As we age, conditions like arthritis, spinal problems, and nerve pain become more common. Pain is real, and it deserves attention. But the way the healthcare system often responds is to move very quickly to strong medications—and escalate doses when relief is incomplete.
Commonly used drugs include:
- Opioids (narcotics)
- Medications like gabapentin or pregabalin
- High-dose anti-inflammatory drugs (NSAIDs)
These medications rarely address the underlying cause of pain. Instead, they act on the nervous system, changing how the brain perceives pain signals. The body adapts, and over time it may take higher and higher doses to get the same effect. This can set up a dangerous cycle of dependence and side effects.
In hospital settings, it’s not unusual to see adults over 75 on large doses of pain medication. The consequences can be dramatic:
- Excessive drowsiness
- Increased confusion or delirium
- Higher risk of falls and injuries
- Loss of engagement with family and daily life
It’s very telling when, for medical reasons, these drugs are reduced or paused. Family members will often say something like:
“Wow, I haven’t seen Mom this alert and clear in years.”
Often, the only thing that changed was less sedating medication.
Even supposedly “routine” treatments like high-dose NSAIDs (e.g., ibuprofen, naproxen) are not harmless. They can cause:
- Bleeding stomach ulcers
- Kidney problems
- Worsening blood pressure control
So before jumping to “big gun” pain medications, it’s worth asking:
- Has physical therapy been fully tried and continued long enough?
- If extra weight is worsening joint pain, has weight loss been strongly supported with realistic strategies?
- Have safer options been explored first, such as:
- Heat and cold therapy
- Gentle exercise and stretching programs
- Occupational therapy
- Braces, supports, or assistive devices
- Appropriately supervised complementary approaches (e.g., acupuncture, massage, mindfulness-based pain management)
Powerful drugs have a place—especially for severe or acute pain—but they should not automatically be the first or only solution, particularly in older adults.
How to Be an Active Partner in Your Healthcare
The most important message is this: you are not powerless in your medical care, even as you age. Overtreatment is often driven by habit, guidelines designed for younger people, time pressure, and a culture that values “doing more” over “doing what’s appropriate.”
To protect your health:
-
Ask Critical Questions
- Why am I taking this medication?
- How clear is the evidence for someone my age?
- What are the realistic chances it will help me?
- What side effects should I watch for?
-
Bring Data, Not Just Symptoms
- Track blood pressure at home.
- Note when dizziness, confusion, or extreme sleepiness occurs.
- Record pain levels, activity, and any changes when medications are adjusted.
-
Discuss Deprescribing
- Ask your doctor whether any medications can be reduced, simplified, or stopped safely.
- Focus especially on:
- Multiple blood pressure drugs
- High-dose statins in very old age
- Long-term opioid or sedating pain medications
-
Focus on Quality of Life
- Treatment should support your ability to think clearly, move safely, enjoy relationships, and live as independently as possible—not just produce “better” lab numbers.
By understanding the risks of overtreatment in high blood pressure, cholesterol management, and chronic pain, you can have more meaningful conversations with your healthcare provider and make decisions that truly align with your health, your age, and your life goals.