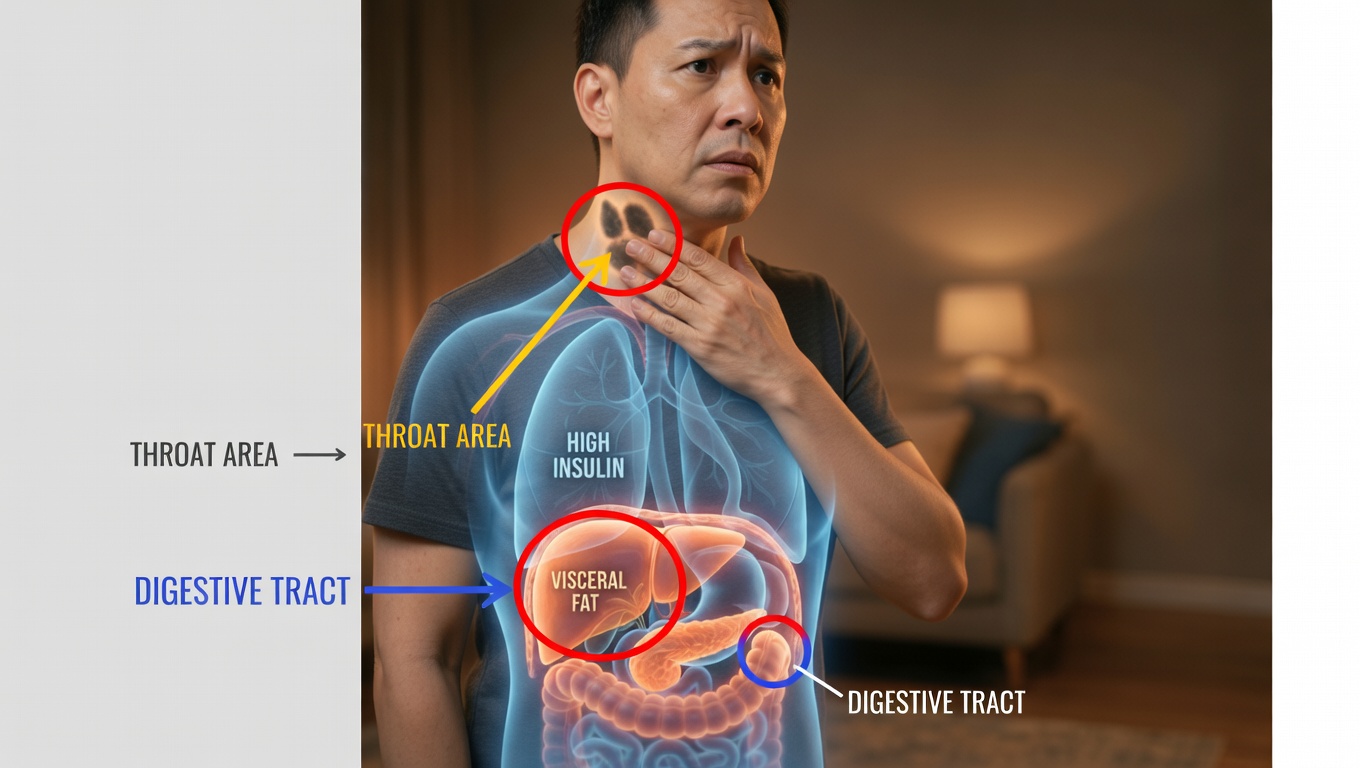
Is Your Body Sounding the Alarm? Hidden Signs of Insulin Resistance
Glance in the mirror or run your fingers along your neck. Do you notice tiny bumps or new skin tags that seemed to appear out of nowhere? Maybe the folds of your skin look darker, almost like stubborn dirt that won’t wash off no matter how hard you scrub. Or perhaps your belly feels firm and protruding, and your abdominal fat refuses to budge despite dieting and “eating healthy.”
This is not about being dirty, lazy, or “just getting older.” These are often early warning signs that your metabolism is struggling with a condition called insulin resistance.
When you are insulin resistant, your body behaves as if it has stopped listening to you and starts storing fat—especially around your waist—as if it were in survival mode. The encouraging news is that insulin resistance is not a life sentence. It can often be improved, and in many cases reversed, with the right strategy.
Based on the insights of Dr. Alberto Sanagustín, we’ll explore why your cells have become “deaf” to insulin and how a simple “silence therapy” can help them tune in again so you can regain control of your weight, energy, and long‑term health.
Key Takeaways
-
What is Insulin Resistance?
A metabolic condition where your cells no longer respond properly to insulin, causing elevated blood sugar and promoting fat accumulation, especially around the abdomen. -
Typical Warning Signs:
- Small skin tags (acrochordons) around the neck, armpits, or under the breasts
- Dark, velvety skin patches in body folds (acanthosis nigricans)
- A hard, protruding belly due to visceral abdominal fat
-
How to Improve It (the “Silence Therapy”):
- Reduce how often you eat to lower frequent insulin spikes
- Change the order in which you eat foods (fiber and protein first, carbs last)
- Do light physical activity, such as a short walk, right after meals
1. What Is Insulin Resistance? The Postman and the Fed‑Up Neighbor
To really understand why weight loss feels impossible and why these skin changes are appearing, let’s skip the usual textbook explanation and use a different image.
Imagine each of your body’s cells is like a neighbor relaxing at home. Insulin is the postman, and glucose (sugar from your food) is the package that needs to be delivered for energy.
How It Used to Work
Decades ago, the postman showed up roughly three times a day:
- He rings the bell at breakfast. The neighbor opens the door, takes the package (glucose), and uses it for energy.
- Same thing at lunch and dinner.
- The visits are spaced out, everyone’s happy, and the system works smoothly.
What Happens Today
Now picture what happens with modern eating habits:
- 8 a.m.: sweet breakfast or pastries
- 11 a.m.: sugary coffee or snack
- 2 p.m.: bread, desserts, or fast food
- 5 p.m.: snack again
- 9 p.m.: big dinner, maybe followed by something sweet
The postman is ringing the bell all day long.
Eventually, the neighbor has had enough. He wants peace and quiet, so he:
- Puts in earplugs
- Stops answering the door
- Ignores the doorbell completely
This is insulin resistance. Your cells are not “broken”; they’re protecting themselves from constant stimulation. They start ignoring insulin because it shows up too often and too loudly.
The Critical Pre‑Diabetes Stage
At this stage, you might not have full-blown diabetes yet, but you’re in a metabolic danger zone. Here’s what happens behind the scenes:
- Your pancreas notices the cells aren’t “opening the door.”
- It assumes insulin isn’t loud enough.
- So it sends more postmen—producing even higher levels of insulin.
Now your blood is crowded with insulin (hyperinsulinemia), but your cells are still resisting and not getting enough usable energy. The result:
- You feel constantly hungry or never fully satisfied.
- You feel tired and drained, even though your body is actually surrounded by stored energy (fat).
Your body is not betraying you—it’s simply trying to cope with the nonstop noise by tuning it out.
2. Three Telltale Signs Your Body Is Asking for Help
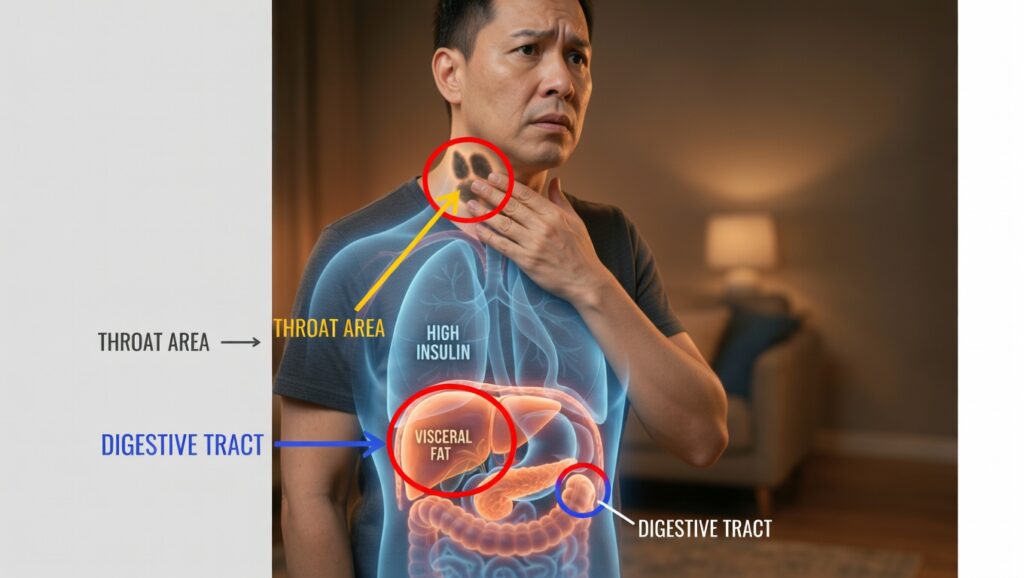
So how do those bumps on your neck and the dark patches on your skin fit into this picture?
When insulin levels stay high for years, that excess insulin starts acting on tissues it normally wouldn’t. It can stimulate skin growth and pigment changes, and it encourages dangerous fat storage deep in your abdomen.
Here are three key signs to look for.
Signal #1: Skin Tags (Acrochordons)
Skin tags are:
- Small, soft, flesh-colored growths
- Commonly found on the neck, armpits, or under the breasts
Medically, they’re usually harmless. However, from a metabolic perspective, they can be viewed as a footprint of chronically elevated insulin. Their appearance—especially when new and multiple—can be a visible clue that your body is wrestling with insulin resistance and underlying metabolic stress.
Signal #2: Acanthosis Nigricans (Dark Skin Patches)
Acanthosis nigricans is the medical name for:
- Darkened, velvety, sometimes thick patches of skin
- Typically appearing in skin folds:
- Back of the neck
- Armpits
- Groin or inner thighs
Many people think this discoloration is due to dirt or poor hygiene, but it is not. It’s often a direct skin reaction to chronically high insulin levels.
Important caution:
- If these dark patches appear suddenly, spread rapidly, or are associated with unexplained weight loss, you should see a doctor promptly to rule out other serious conditions.
Signal #3: Hard, Protruding Belly Fat (Visceral Fat)
Not all belly fat is the same. With insulin resistance, you often see:
- A firm, protruding abdomen
- Fat that feels hard rather than soft and squishy
This is visceral fat—fat stored deep inside your abdominal cavity, wrapped around your organs. It is strongly linked to metabolic syndrome, insulin resistance, fatty liver, and cardiovascular disease.
Visceral fat and insulin resistance reinforce each other:
- Visceral fat makes your cells more insulin resistant.
- Insulin resistance encourages your body to store more visceral fat.
These signs are strong clues, but they are not a diagnosis. If you recognize several in yourself:
- Don’t jump to conclusions.
- Schedule an appointment with your healthcare provider.
A simple blood test (including glucose, insulin, and possibly HOMA‑IR or an oral glucose tolerance test) can often detect insulin resistance early and give you a clear picture of your metabolic health.
3. “Silence Therapy”: How to Help Your Cells Hear Insulin Again
If you see yourself in these descriptions, it’s important to know you’re not powerless. Many people can improve insulin sensitivity significantly by changing daily habits, not just relying on medication.
The goal of “Silence Therapy” is to turn down the metabolic noise—to give your cells long enough breaks from insulin so they can start responding normally again.
This strategy has three main steps.
Step 1: Give the Doorbell a Break (Reduce Meal Frequency)
Every time you eat—especially carbohydrates—your body releases insulin. If you’re eating or snacking five or six times a day, you’re pressing that doorbell constantly.
To reduce the noise:
- Aim for 2–3 satisfying, nutrient-dense meals per day instead of constant grazing.
- Leave 4–5 hours between meals so insulin has time to drop back down.
This is not about extreme fasting or starving yourself. It’s about:
- Eating enough at each meal
- Choosing foods that keep you full longer (protein, healthy fats, fiber)
- Avoiding mindless snacking between meals
Also, try to remove the loudest “noisemakers”:
- Sugary drinks (sodas, juices, energy drinks, sweetened coffees and teas)
- Alcohol, especially in frequent or high amounts
These act like holding a megaphone to your cell’s ear—huge insulin spikes in a short time. Minimizing or eliminating them, especially during your “therapy period,” can speed up improvement in insulin sensitivity.
Important medical warning:
If you have diabetes and use insulin or other blood sugar-lowering medications, do not change your meal timing or frequency without medical supervision. Longer gaps between meals can lower your blood sugar and may require adjustment of your medication. Always consult your doctor first.
Step 2: Use the “Butler’s Trick” (Change the Order of Your Food)
This strategy is simple but powerful: the order in which you eat your food matters.
Instead of starting your meal with the loudest “postmen” (starches and sugars), you send in the quietest ones first:
- Begin with fiber-rich vegetables (salad, cooked veggies, soup with vegetables).
- Then eat your protein and healthy fats (meat, fish, eggs, tofu, legumes, olive oil, avocado, nuts).
- Finish with your starches or carbohydrates (rice, pasta, bread, potatoes, dessert).
Why this works:
- Fiber and protein slow stomach emptying and digestion.
- This leads to a smaller and slower rise in blood sugar.
- As a result, the insulin spike is lower, even if you eat the same amount of carbohydrates.
Research shows that simply eating carbohydrates at the end of the meal can significantly reduce the post-meal insulin and glucose response. Same foods, same calories—just less metabolic noise.
Step 3: Open the Service Door (Move After You Eat)
This is one of the most underrated tools for improving insulin resistance and fatty liver: light movement after meals.
If you walk for just 10–15 minutes immediately after eating, you:
- Help your muscles absorb more glucose
- Allow sugar from your meal to enter cells with less need for insulin
- Reduce blood sugar spikes and support better insulin sensitivity over time
Think of it as opening a “service entrance” directly into your muscles. Instead of insulin shouting at the front door, your muscles quietly take in glucose through movement.
You don’t need intense exercise:
- A relaxed walk around the block
- Light housework
- Gentle cycling
Consistency matters more than intensity. Doing this after your main meals can make a noticeable difference in how your body handles glucose.
Putting It All Together
Skin tags, dark patches on your neck, and a hard, rounded belly are not just cosmetic concerns or signs of aging. They can be early signals of insulin resistance—your body’s way of saying that your metabolism needs attention.
By:
- Reducing how often you eat and cutting out constant snacking
- Changing the order in which you eat your food (fiber and protein first, carbs last)
- Adding light movement right after meals
you can begin to lower the metabolic “noise” and help your cells “hear” insulin again.
If you recognize these signs in yourself:
- Talk with your doctor and request appropriate blood tests.
- Start applying these simple lifestyle changes as part of a long-term plan to protect your health.
Insulin resistance is often reversible, especially when caught early. Your body has been sending you signals—now is the time to listen and respond.