A New Clue in Alzheimer’s Disease and Vascular Dementia
Researchers at Oregon Health & Science University have identified a newly recognized way brain cells may die in Alzheimer’s disease and vascular dementia. This finding offers a fresh way to think about how these conditions progress and may help guide future treatment research.
The study, published in Annals of Neurology, points to ferroptosis as a key process involved. Ferroptosis is a form of cell death triggered by the buildup of iron inside cells. In this case, researchers found it may be responsible for the loss of microglia in the brain.

The Problem: Microglia Are Dying in Key Brain Areas
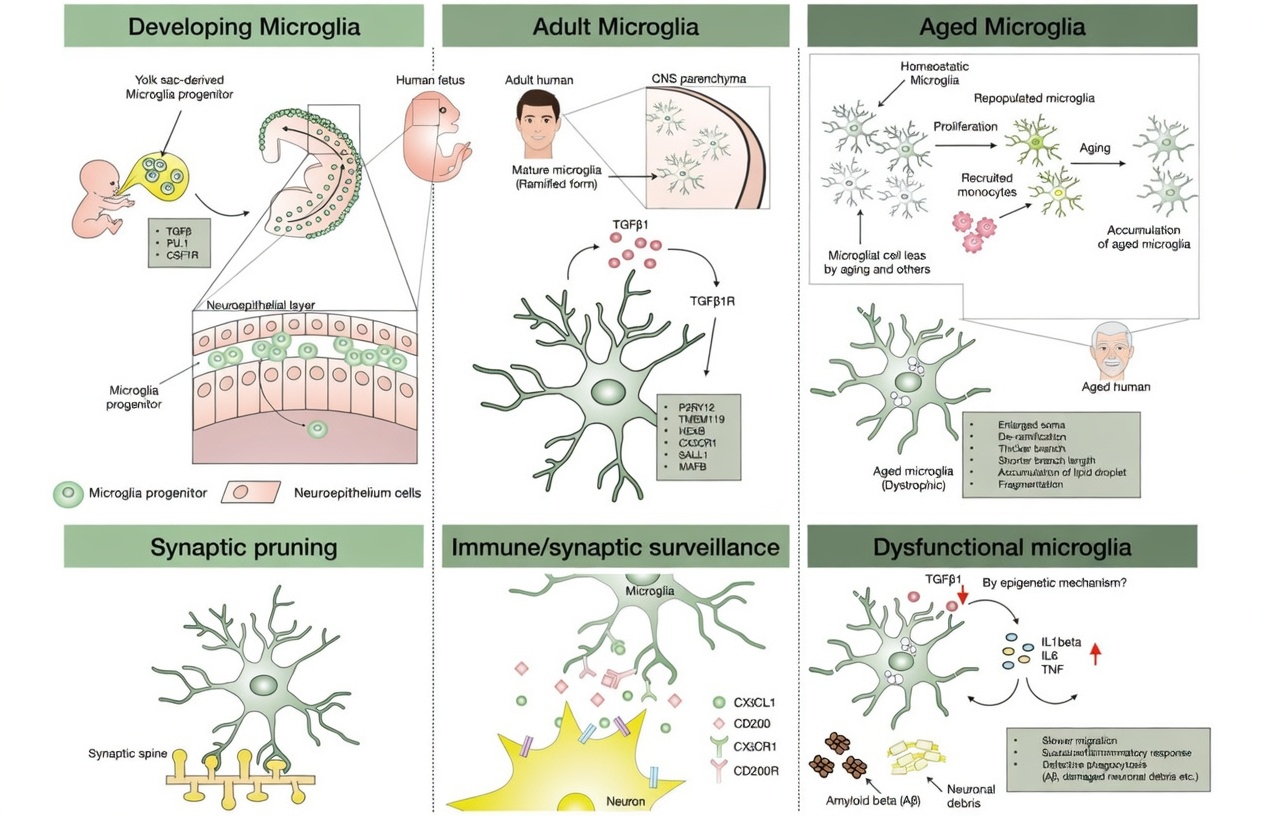
Microglia are the brain’s resident immune cells. They help keep the brain healthy by clearing away cellular debris, especially when myelin is damaged. Myelin is the protective covering around nerve fibers, and it plays an important role in brain function.
The researchers discovered that in the white matter of the brains of people with Alzheimer’s disease and vascular dementia, microglia were degenerating. This matters because these cells normally serve a protective role. If they are lost, the brain may become less able to manage damage, which could contribute to cognitive decline.
Stephen Back, M.D., Ph.D., a neuroscientist and professor of pediatrics in the OHSU School of Medicine, described the finding in striking terms, saying, “We’ve missed a major form of cell death in Alzheimer’s disease and vascular dementia. It’s just amazing that we missed this until now.”
The Cause: Iron-Rich Myelin May Trigger Ferroptosis
According to the study, the problem may begin when microglia clean up iron-rich myelin. While this cleanup is meant to protect the brain, the process may expose microglia to iron toxicity. As iron builds up in these cells, it can trigger ferroptosis and lead to their destruction.
This changes how researchers understand neurodegeneration in Alzheimer’s disease and vascular dementia. Instead of simply viewing microglia as defenders, the study suggests these cells may die while carrying out their normal protective job.
The research team, led by senior author Stephen Back, used innovative methods that included examining post-mortem brain tissue from people with dementia. Lead author Philip Adeniyi, Ph.D., a postdoctoral researcher in Back’s laboratory, developed the technique that helped reveal what was happening in white matter regions of the brain.
Co-author Kiera Degener-O’Brien, M.D., observed the degeneration of microglia, supporting the idea that myelin fragments and iron toxicity may be driving this process.
The study also suggests that this damaging cycle may begin with repeated periods of reduced blood flow and lower oxygen supply to the brain. Acute stroke may play a role, and chronic conditions such as hypertension and diabetes may also contribute.
The Solution: New Directions for Dementia Research and Treatment
This discovery may open the door to a new direction in dementia research. By identifying microglial degeneration and ferroptosis as part of the disease process, scientists may be better able to explore ways to protect these cells.
Dr. Back said he expects the pharmaceutical industry to take interest in developing compounds aimed at microglial degeneration. That could create new possibilities for future therapies in Alzheimer’s disease and vascular dementia.
He also emphasized that dementia develops over many years, making early attention especially important: “Dementia is a process that goes on for years and years. We have to tackle this from the early days to have an impact so that it doesn’t spin out of control.”
Why This Discovery Matters
This finding gives researchers a new framework for understanding how dementia may worsen over time. By focusing on ferroptosis and the loss of microglia in white matter, the study adds important detail to the bigger picture of Alzheimer’s disease and vascular dementia.
While more work is still needed, this breakthrough brings new energy to the field and may shape future research, drug development, and dementia care.
Consult a healthcare professional before making changes.



