Why Understanding Your Blood Pressure Really Matters as You Get Older
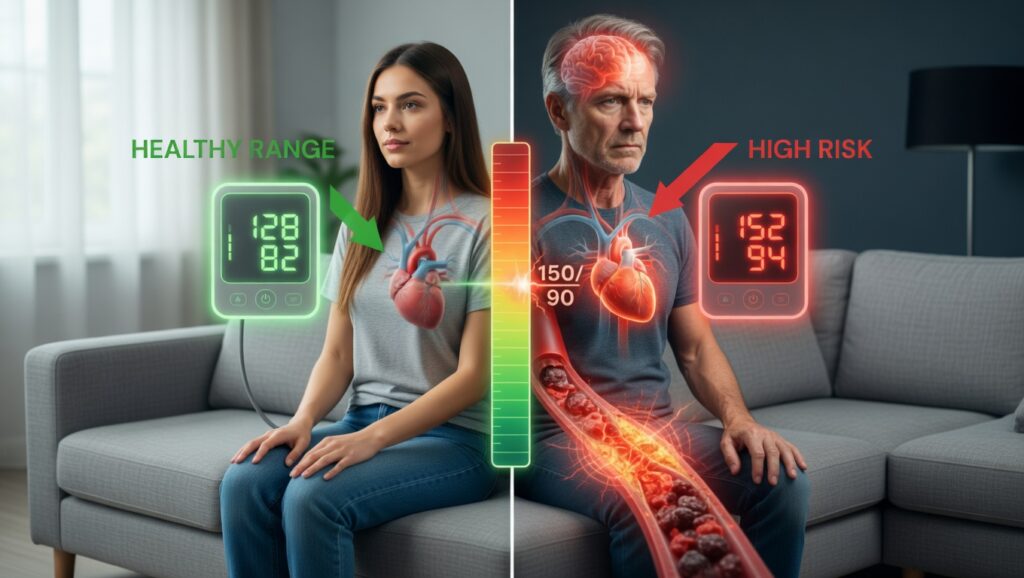
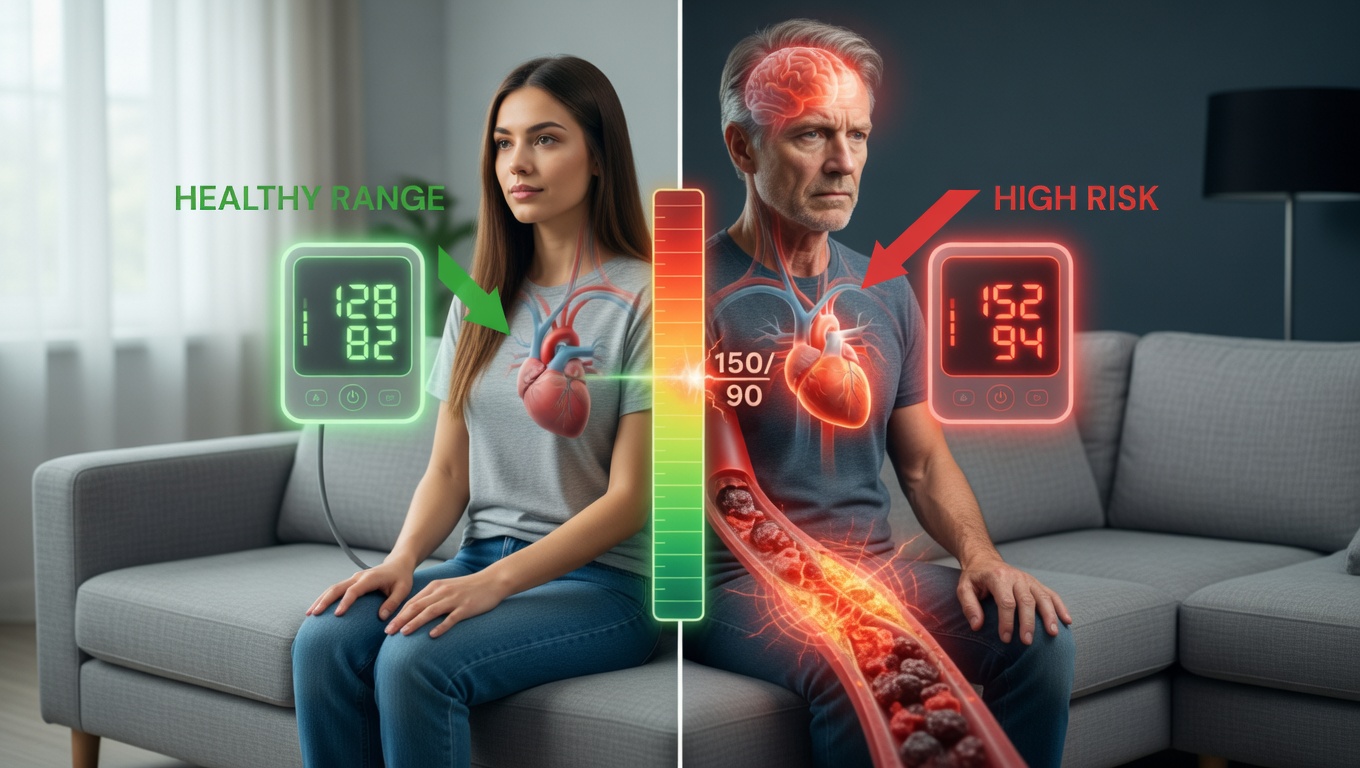
If you want to protect your heart, brain, and independence as you age, you need to know what your blood pressure readings actually mean. Many people—especially older adults—are unsure which numbers are truly worrisome. One person is told a high reading is “normal for your age,” while another is put on extra medication for a similar result. It’s no surprise you’re left wondering: is this number dangerous or not?
Blood pressure is not a simple “good” or “bad” number, and the rules change somewhat as we get older. For years, medical advice was inconsistent. At one time, doctors even used a rule of thumb that said your “normal” top number (systolic) could be 100 plus your age—so a reading of 180 might have been accepted in an 80-year-old. We now know that is too high and increases your risk of stroke, heart attack, and kidney damage.
On the other hand, trying to force every slightly elevated reading down with medication is not always wise either. To make sense of it, you need to understand what the numbers represent, how blood pressure naturally changes throughout the day, and how to measure it correctly. This guide, based on the insights of Dr. Mitch Rice, will help you do exactly that so you can manage your health with clarity instead of fear.
Key Takeaways
-
Know the two numbers:
Blood pressure readings have a top number (systolic) and a bottom number (diastolic).- Systolic = pressure when your heart contracts.
- Diastolic = pressure when your heart relaxes between beats.
Both matter, but they tell different parts of the story.
-
Context is crucial:
A single high reading is not a diagnosis of hypertension. Blood pressure naturally goes up and down with activity, stress, talking, and daily life. Doctors look for a pattern, not one-off spikes. -
Accurate measurement is essential:
Your “real” blood pressure is your resting blood pressure, measured correctly and consistently over weeks. Quick checks in a busy clinic or right after walking in are often misleading. -
What counts as “too high” depends on age and pattern:
- For most people over 60, consistent resting readings above 150 systolic or 90 diastolic are considered too high and need attention.
- For younger adults, concern usually begins around 140/85 at rest.
-
Pay attention to symptoms:
Shortness of breath, chest pain, severe headache, dizziness, or feeling faint are warning signs, even if your numbers don’t look extreme. If you feel unwell, seek medical advice promptly.
1. The Two Blood Pressure Numbers: Systolic vs. Diastolic
Every blood pressure reading has two values, such as 130/80. Each number reflects a different part of your heart’s pumping cycle:
-
Systolic (top number):
This is the highest pressure in your arteries when your heart contracts and pushes blood out. Imagine a strong wave hitting the shore—that’s the peak force on your artery walls. As we age, our arteries typically become stiffer, so the systolic number often rises gradually. A modest increase is common and not always dangerous, but a consistently high systolic pressure does increase risk over time. -
Diastolic (bottom number):
This is the pressure in your arteries when your heart relaxes between beats and refills with blood. It represents the ongoing, steady pressure in your blood vessels all the time. Diastolic pressure is less about the “surge” and more about constant strain.
Both numbers are important, but they behave differently with age. In older adults, the systolic number often climbs while the diastolic number may stay the same or even drop slightly. Understanding this helps you interpret your readings more accurately.
2. Understanding Your Systolic (Top) Number
Your systolic number is often the one doctors focus on most, especially in people over 60. Here is a simple guide to interpreting it at rest:
-
Below 120:
- Generally considered optimal.
- Associated with the lowest long-term risk for heart disease and stroke.
-
120 to 129:
- Still a healthy and acceptable range for most people.
- Worth maintaining with a balanced lifestyle.
-
130 to 139:
- In older adults (over 60), this may be a very reasonable range, particularly if you feel well, remain active, and have no major health problems.
- It’s a “monitor closely” range, not an automatic “start more medication” zone.
-
140 to 149:
- This range signals that something needs attention.
- It does not necessarily mean you must start or increase medication immediately, but it is a clear sign to:
- Review your diet (salt, alcohol, processed foods).
- Look at stress, sleep, and physical activity.
- Check that you’re measuring blood pressure correctly.
-
150 and above:
- If your readings are consistently 150 or higher at rest, this is considered too high for most people.
- This level of ongoing pressure puts a heavy load on your heart, brain, and kidneys and significantly increases cardiovascular risk.
A key takeaway: a systolic reading in the 130s or low 140s, especially in someone over 60 who feels well and is functioning independently, is usually not an emergency. What really matters is the pattern over time, how often the readings are elevated, and whether they stay high even at rest.
3. Understanding Your Diastolic (Bottom) Number
Your diastolic number reflects the continuous pressure on your arteries. Persistent elevation here is a serious concern, particularly in middle-aged and younger adults.
Here’s how to think about diastolic readings at rest:
-
Below 80:
- Generally ideal and associated with lower cardiovascular risk.
-
80 to 84:
- Very common and usually acceptable for most people.
-
85 to 89:
- A “watch closely” zone.
- Not necessarily dangerous by itself, but it’s a signal to monitor your blood pressure pattern more carefully.
-
90 and above:
- If your diastolic pressure is 90 or higher consistently at rest, it deserves serious attention.
- This means your arteries are under high pressure all the time, even when your heart is in its resting phase, which can gradually damage blood vessels and organs.
Putting systolic and diastolic together, most experts—and Dr. Rice—consider resting readings of 150+ systolic and/or 90+ diastolic to be too high for the majority of people and a clear reason to take action with lifestyle changes and, if needed, medical treatment.
4. The Golden Rule: Readings Must Be “At Rest”
The most important principle—and the one most often overlooked—is this:
Your blood pressure should be judged based on readings taken when you are fully at rest.
A number like 150 taken:
- After rushing to an appointment
- Following a stressful phone call
- Immediately after climbing stairs
- While you are anxious in a doctor’s office
does not represent your true baseline blood pressure. That is your reactive blood pressure—your body’s normal response to stress or activity.
To know whether your blood pressure is genuinely too high, you need:
- Calm conditions
- A consistent method
- Readings collected over several days or weeks
Without this, individual readings can be misleading and may result in unnecessary worry or overtreatment.
5. How to Measure Your Blood Pressure Correctly at Home
To discover your real baseline blood pressure, it’s essential to follow a careful routine every time you check it. This reduces the chance of artificially high numbers and gives your doctor reliable data.
Use this step-by-step protocol:
-
Sit quietly first:
- Sit in a comfortable chair with your back supported for 5 full minutes.
- Do not talk, read, or scroll on your phone. Just relax and breathe normally.
-
Position your body correctly:
- Keep both feet flat on the floor.
- Do not cross your legs.
- Rest your arm on a table or armrest so that the cuff will be at heart level.
-
Empty your bladder:
- A full bladder can raise your reading by several points, giving a false impression of high blood pressure.
-
Take two readings:
- Take the first measurement.
- Wait one minute.
- Take a second measurement.
-
Record the lower value:
- Write down the lower of the two readings.
- That lower reading is your value for that session.
Additional tips:
- Use a validated, upper-arm automatic blood pressure monitor, not a wrist or finger device.
- Measure twice a day:
- Once about 20 minutes after waking up (before caffeine or heavy activity).
- Once as the last thing you do before going to sleep.
- Alternate arms each day (left one day, right the next).
After one week, you’ll have about 14 readings. Calculate the average of those readings. That average is the best estimate of your true baseline blood pressure and is what you and your doctor should use to make decisions.
6. Why Blood Pressure Spikes Happen—and Why Not to Panic
Blood pressure is not a fixed number; it is meant to change throughout the day. Variations of 20 to 40 points or more are often completely normal. This is your body adapting to what you are doing and feeling.
Your blood pressure naturally rises with:
- Physical movement or exercise
- Stress, anxiety, or anger
- Pain
- Excitement or strong emotions
- Caffeine or nicotine
- Cold temperatures
- Talking or being active during the measurement
It naturally falls with:
- Rest and relaxation
- Deep, calm breathing
- Warmth and comfort
- Sleep
So, seeing a reading of 145 midday during a hectic schedule and 126 in the evening while resting on the couch can be entirely normal for the same person.
The key principle:
We don’t treat isolated spikes; we treat sustained, consistently high patterns at rest.
By focusing on accurately measured, resting blood pressure over time, you can avoid unnecessary fear about normal fluctuations and concentrate on what truly matters for protecting your heart, brain, and long-term independence.