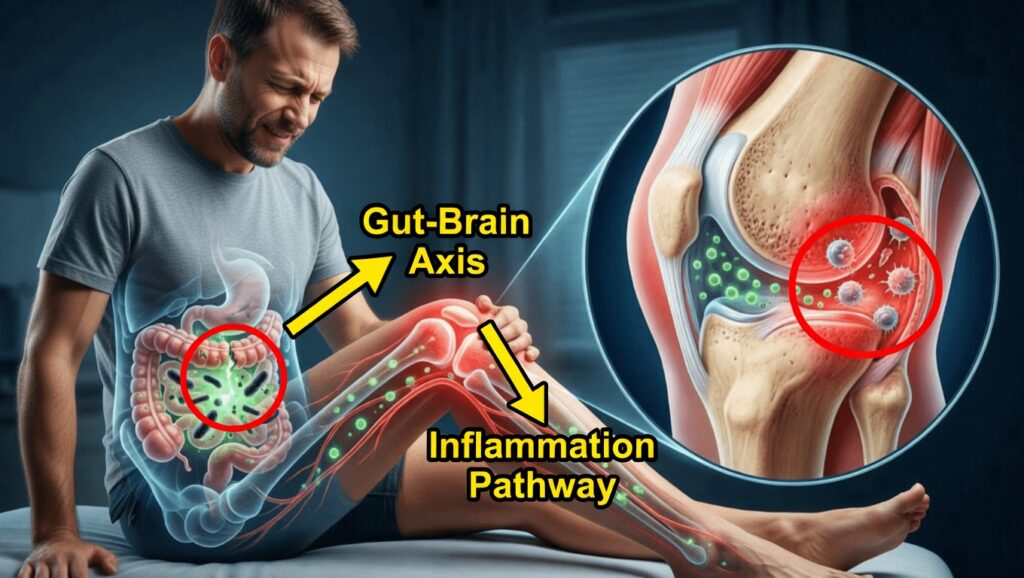
Is Your Knee Pain Really Just “Wear and Tear”? Think Again
Are you exhausted from hearing the same answer every time you see a doctor about your joint pain?
“It’s the weather.”
“It’s your age.”
“It’s just wear and tear.”
In many cases, that explanation is incomplete—or simply wrong.
If you suffer from chronic pain in your knees, hips, or hands; if your joints are swollen, inflamed, or you’ve been told you have osteoarthritis, one major underlying cause may be something completely different: intestinal hyperpermeability, more commonly known as leaky gut.
We’re often told joint pain is an unavoidable part of getting older. But at what point did we decide that time itself is the culprit, instead of looking deeper at how our metabolism and lifestyle are affecting our bodies?
You might think you “eat pretty well,” with the occasional treat that slowly becomes a daily habit. Meanwhile, your metabolism is under constant attack—and your reflection in the mirror is not just cosmetic feedback; it’s a direct signal of your metabolic health.
This metabolic chaos has a powerful impact on your joints, particularly your knees, and it affects women in unique ways. The following insights draw on the work of Dr. Javier Furman.
Key Takeaways
-
Stop Blaming Age Alone: Joint pain usually isn’t just a consequence of getting older, gaining weight, or “wearing out” your joints. Those issues are often symptoms, not the real source of the problem.
-
Your Gut Talks to Your Knees: A leaky gut allows bacterial toxins to slip through your intestinal lining into your bloodstream, creating systemic inflammation.
-
Targeted Damage in the Knees: These toxins have a strong attraction to the synovial lining of the knee joint, where they can trigger an autoimmune reaction—your immune system begins attacking your own joint tissue.
-
Real Relief Starts in the Gut: Long-term improvement doesn’t come from a single pill or injection. It comes from healing your gut, supporting your liver, and living in a way that calms inflammation throughout your body.
1. It’s Not Your Age – It’s Your Gut
Blaming your birthdays for your pain is an oversimplification that ignores the complex biology inside you.
For women, the story is even more layered. Their hormonal system is more intricate than men’s and they:
- Carry the physical demands of pregnancy,
- Endure childbirth,
- Breastfeed,
- And then face menopause, often around age 50, with a dramatic shift in estrogen levels.
These hormonal changes can significantly influence bone density, cartilage health, and joint structure—making women more vulnerable to osteoarthritis and joint pain. It’s not that women are more fragile or less tolerant of pain. In fact, many women tolerate pain remarkably well, but their physiology comes with unique challenges.
The Microbiome and Hormones
This is where the gut steps in.
Inside your intestines lives a massive community of microbes called the gut microbiome. Among these bacteria, women have a special subgroup known as the estrobolome, a collection of microbes specifically involved in metabolizing and regulating estrogen.
When gut health deteriorates—due to diet, stress, medications, or infections—this delicate microbial ecosystem is disrupted. That imbalance can throw estrogen metabolism out of alignment, affecting joints, bones, and overall inflammation.
And the problem is not limited to women. A compromised gut can drive chronic inflammation and joint damage in everyone, regardless of gender.
2. What Is Leaky Gut and How Does It Harm Your Knees?
Picture your intestinal lining as a fine mesh or filter. Its job is to:
- Allow digested nutrients (like vitamins, minerals, amino acids, and healthy fats) to pass into your bloodstream,
- Block larger, harmful particles such as toxins, undigested food, and bacteria.
In a healthy gut, the junctions between intestinal cells are tight and selective.
With leaky gut (intestinal hyperpermeability), those junctions loosen. The “mesh” becomes porous.
How It Starts: Dysbiosis and Toxic Bacteria
When the balance of your gut microbiome is disturbed—a situation called dysbiosis—harmful bacteria can overgrow. These bacteria produce a toxic substance called lipopolysaccharides (LPS).
LPS is especially dangerous because it:
- Damages the proteins that hold intestinal cells together,
- Creates microscopic gaps in the gut barrier,
- Allows LPS and other bacterial fragments to leak directly into your bloodstream.
At that point, your gut’s protective wall has been breached, and your immune system sees these invaders as a serious threat.
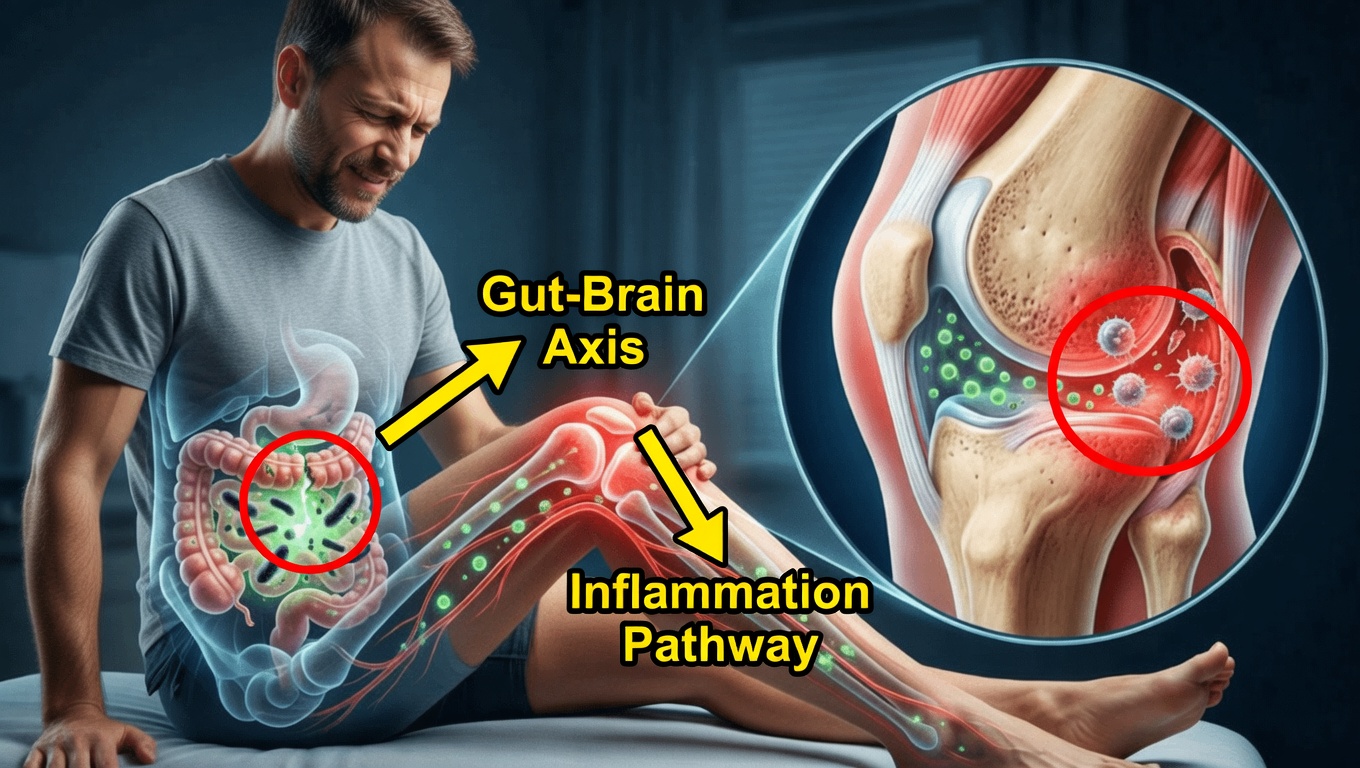
3. From Gut to Knee: The Toxic Journey
Once bacterial toxins like LPS enter the bloodstream, your liver becomes the primary defender. Its job is to neutralize and eliminate these toxins.
However, a modern diet overloaded with:
- Refined carbohydrates,
- Processed foods,
- Sugary drinks,
- Alcohol,
places the liver under relentless stress. Over time, it becomes overwhelmed and less efficient at detoxifying the blood.
When the liver can’t keep up, LPS and other toxins continue circulating, creating a low-grade, chronic inflammatory state known as metabolic endotoxemia.
Why Your Knees Take the Hit
Here’s where it gets crucial for joint health:
- LPS has a particular attraction to the synovial membrane, the tissue that lines and lubricates your knee joint.
- These toxins accumulate in the synovial capsule.
- Your immune system identifies LPS as foreign and mounts an attack.
The problem? The immune system can’t clearly distinguish between the toxin and the joint tissue it’s attached to. As a result, it starts attacking the synovial lining itself.
This is an autoimmune process: your body’s own defense system is creating the inflammation, swelling, and pain in your knee—then we casually label it as “wear and tear.”
4. Why Exercise Sometimes Makes Your Knees Hurt More (At First)
Maybe you’ve experienced this scenario:
You’ve been inactive and not eating well. Motivated to change, you decide to go for a long walk or start an exercise routine. Instead of feeling better, your knees are throbbing afterward. You conclude, “Exercise is bad for me,” and go back to being sedentary.
Here’s what’s really going on.
The Knee’s Unique Blood Supply
The knee joint is unusual in that it has a very limited direct blood supply. If you opened up the joint, you’d notice it appears almost entirely white—there are very few blood vessels.
So how does it receive nutrients?
Through a process called imbibition, where:
- Movement acts like a pump,
- Fluid from the surrounding tissues is squeezed into and out of the joint,
- Nutrients and waste products are exchanged through this movement-driven flow.
Now imagine this:
If the fluid surrounding your joint is loaded with inflammatory toxins from a leaky gut, each step you take is essentially pumping irritants into your knee. You’re bathing your joint in an inflammatory cocktail.
Your immune system, already on high alert, responds with even more aggression. The result is:
- Increased pain,
- More stiffness,
- A feeling that movement is making things worse.
Exercise itself is not the enemy. The problem is the toxic internal environment you’re moving in. You need to clear the metabolic chaos first so that movement becomes healing instead of harmful.
5. A 4-Week Plan to Start Reclaiming Your Knees
There is no single supplement, injection, or medication that can instantly erase years of metabolic damage. Real, lasting improvement comes from supporting your body’s natural healing systems—especially the gut and liver.
Think of your liver as the key organ, and your gut as the doorway to joint recovery.
Commit to a 4-week anti-inflammatory reset. Four weeks is enough to feel a noticeable difference.
Step 1: Remove Major Inflammatory Triggers
For the next 4 weeks, completely avoid:
- Refined flours (white bread, pastries, crackers, etc.)
- Gluten-containing grains (wheat, barley, rye)
- Added sugars and sugary drinks
- Dairy products (especially milk, ice cream, soft cheeses)
- Alcohol
No exceptions during this period.
These foods:
- Feed harmful gut bacteria,
- Worsen dysbiosis,
- Increase intestinal permeability,
- Promote systemic inflammation.
Instead, focus on:
- High-quality proteins: fish, eggs, poultry, grass-fed meat, legumes (if tolerated)
- Healthy fats: olive oil, avocado, nuts, seeds, fatty fish
- Plenty of vegetables: aim for a wide variety of colors and types
- Low-glycemic fruits: berries, apples, pears in moderation
Step 2: Support Your Liver
By removing inflammatory and toxic foods, you give your liver a chance to shift from constant crisis management to deep detoxification.
This allows it to:
- Process and eliminate built-up toxins more efficiently,
- Reduce the burden of circulating LPS,
- Lower systemic inflammation that affects your joints.
You can further help your liver by:
- Staying well-hydrated with water and herbal teas,
- Avoiding unnecessary medications when possible (only under medical guidance),
- Eating bitter and sulfur-rich foods (like arugula, dandelion greens, garlic, onions, broccoli, and Brussels sprouts).
Step 3: Move—But Gently at First
During these initial 4 weeks, choose low-impact activities that:
- Encourage circulation,
- Avoid excessive pounding on your joints.
Good options include:
- Swimming or water aerobics
- Cycling or stationary bikes
- Gentle yoga or mobility work
After your body has had time to reduce inflammation and begin healing, you can gradually introduce:
- Walking,
- Light strength training,
- More dynamic exercises,
always increasing intensity progressively and listening to your body’s signals.
Step 4: Prioritize Deep, Restorative Sleep
Your joints, especially your knees, do most of their repair and regeneration while you sleep.
Aim for:
- 7–9 hours of quality sleep each night,
- A cool, dark, quiet bedroom,
- Consistent sleep and wake times.
Good sleep is not optional if you’re serious about healing—it’s one of the most powerful anti-inflammatory tools you have.
6. Helpful Supplements to Support the Process
Diet and lifestyle changes are the foundation. Supplements can be useful adjuncts, but they are not a replacement for the work you do with food, movement, and sleep.
Consider these as potential helpers (always check with a healthcare provider before starting new supplements):
L-Glutamine
- An amino acid that serves as the primary fuel source for cells lining the intestines.
- May help repair and tighten the junctions between intestinal cells, supporting the healing of a leaky gut barrier.
Undenatured Type II Collagen
- A specific form of collagen that can help promote joint health.
- May support the integrity of cartilage and help modulate the immune response in the joint, potentially reducing pain and stiffness.
High-Quality Probiotics
- Help restore a balanced gut microbiome.
- Can support the estrobolome in women and improve overall gut barrier function.
- Look for multi-strain products with clinically studied bacteria.
Omega-3 Fatty Acids (EPA/DHA)
- Found in fish oil or algae oil supplements.
- Have strong anti-inflammatory properties that can help reduce joint pain and support cardiovascular and brain health.
Curcumin (from Turmeric)
- A plant compound with potent anti-inflammatory and antioxidant effects.
- May help lower systemic inflammation and improve joint comfort when absorbed well (look for formulations with enhanced bioavailability).
Bringing It All Together
Your joint pain—especially in your knees—is often not just a mechanical issue or an inevitable side effect of getting older. It’s frequently the result of a deeper metabolic and inflammatory problem rooted in your gut and liver.
By:
- Removing foods that inflame your gut,
- Supporting your liver’s detoxification,
- Moving gently while your body heals,
- Prioritizing restorative sleep,
- Using targeted supplements as support,
you give your body a genuine chance to reduce inflammation, protect your joints, and experience less pain.
Your knees are not simply “worn out.” In many cases, they’re under attack from within—and you have the power to change that starting in your gut.