Sjogren’s Syndrome: 13 Warning Signs You Shouldn’t Ignore
Feeling exhausted all the time, dealing with unexplained joint pain, or told that your dry eyes and mouth are “just allergies” or “getting older”? These could be more than minor annoyances. For many people, they are early clues of Sjogren’s syndrome—an often-overlooked autoimmune disease that affects millions worldwide and is frequently missed or misdiagnosed.
Drawing on insights from rheumatologist Dr. Micah Yu, this guide breaks down the key signs and symptoms so you know what to watch for and when to seek help.
Key Takeaways
- Sjogren’s syndrome is a long-term autoimmune condition that can involve many organs and systems—not only the eyes and mouth.
- Symptoms are often vague and nonspecific, such as fatigue and joint pain, which can delay diagnosis.
- Recognizing the full spectrum of Sjogren’s symptoms helps you and your healthcare team pursue earlier, more targeted treatment.
Below are 13 major signs and symptoms of Sjogren’s syndrome and what each may mean for your health.
1. General Symptoms: Unintentional Weight Loss and Extreme Fatigue
If you feel constantly drained, even after a full night’s sleep, or you’re losing weight without changing your diet or exercise routine, Sjogren’s could be a factor.
- Fatigue can become so intense that ordinary activities—working, doing chores, or even getting out of bed—feel overwhelming.
- Ongoing, unexplained tiredness or weight loss should never be dismissed as “just stress” or “aging.”
Persistent fatigue deserves a thorough evaluation, especially when paired with other symptoms below.
2. Joint Pain, Swelling, and Stiffness
Joint problems aren’t limited to rheumatoid arthritis. Sjogren’s can also cause:
- Aching or tender joints
- Swelling and warmth
- Morning stiffness
- Reduced range of motion
In Sjogren’s, the immune system can mistakenly attack joint tissues. Unlike rheumatoid arthritis, joint damage (erosions) is less common, and symptoms may fluctuate—getting worse during flares and easing at other times.
3. Muscle Pain and Weakness
Between 20–40% of people with Sjogren’s report:
- Muscle aches (myalgia)
- A sense of heaviness or weakness in the arms or legs
- Pain or fatigue in muscles after mild activity
If climbing stairs, lifting objects, or walking short distances feels unusually difficult or painful, talk to your doctor; muscle involvement can be part of the disease.
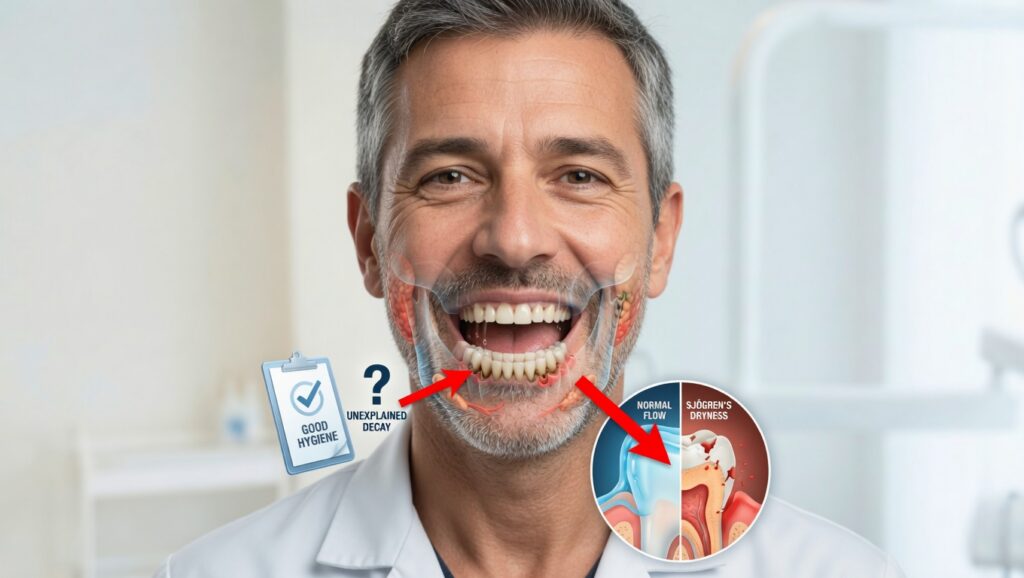
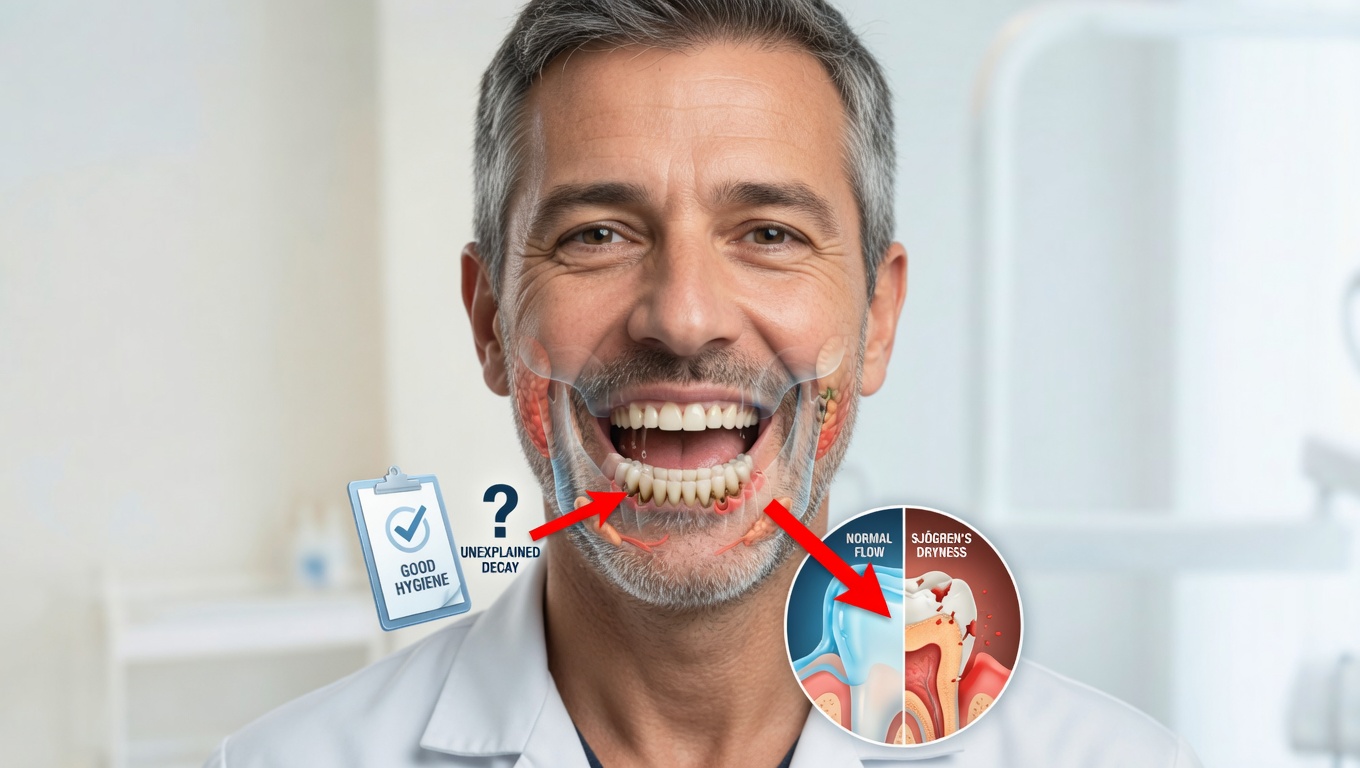
4. Classic Hallmarks: Dry Eyes and Dry Mouth
These are the most recognized Sjogren’s symptoms—and for many, the first to appear. Inflammation targets the glands that produce tears and saliva, leading to:
- Gritty, burning, or “sandy” feeling in the eyes
- Needing eye drops frequently
- Difficulty chewing or swallowing dry foods without sipping water
- Needing water to talk for long periods
- Waking at night because your mouth feels parched
Reduced saliva also raises your risk of cavities, gum disease, and oral infections, so recurrent dental problems can be another clue.
5. Dry, Itchy, or Tight Skin
Sjogren’s doesn’t just dry out your eyes and mouth; it can affect the oil and sweat glands that keep your skin hydrated. You may notice:
- Rough, flaky, or scaly skin
- A tight, stretched feeling
- Itching that regular moisturizers don’t fully relieve
If your skin remains persistently dry despite good skincare and hydration, autoimmune causes should be considered.
6. Vaginal Dryness and Discomfort
This often goes unmentioned, but vaginal dryness is very common in women with Sjogren’s and can affect:
- Everyday comfort
- Sexual intercourse (pain, irritation, or burning)
- Confidence and intimate relationships
Some women find benefit from oil-based suppositories, like coconut oil, or prescription treatments. However, options specifically designed for Sjogren’s-related dryness remain limited, making open discussion with your doctor especially important.
7. Skin Rashes and Vasculitis
Sjogren’s can inflame blood vessels in the skin, a condition known as cutaneous vasculitis. This may appear as:
- Red or purple spots
- Raised bumps or patches
- Rashes that don’t fade or resolve quickly
Any new or persistent rash—especially if it’s painful, doesn’t blanch, or keeps returning—should be evaluated by a dermatologist or rheumatologist.
8. Digestive and Gastrointestinal Problems
Sjogren’s can also involve the digestive tract. Symptoms may include:
- Abdominal pain or cramping
- Bloating and gas
- Chronic diarrhea or loose stools
- Difficulty swallowing (dysphagia)
These complaints are easy to blame on food, infections, or stress. However, ongoing or recurring gut issues should be assessed, particularly if they coexist with other signs of autoimmune disease.
9. Interstitial Lung Disease (ILD)
Around 1 in 5 people with Sjogren’s may develop lung involvement, including interstitial lung disease, where the lung tissue becomes inflamed. Warning signs include:
- Shortness of breath, especially with exertion
- Persistent, dry cough
- Unexplained fatigue or reduced exercise tolerance
Without treatment, chronic inflammation can lead to lung scarring (fibrosis), so early detection is critical.
10. Nervous System Involvement
Sjogren’s can affect both the peripheral nervous system and, less commonly, the central nervous system:
- Numbness, tingling, or burning sensations in hands and feet (neuropathy)
- Weakness or loss of coordination
- Autonomic nerve issues, leading to abnormal heart rate, blood pressure changes, dizziness, or increased anxiety
Because these symptoms overlap with many other conditions, they can be overlooked. A neurologist and rheumatologist working together can help identify whether Sjogren’s is contributing.
11. Raynaud’s Phenomenon
If your fingers or toes change color in the cold—turning white, then blue, then red—you may have Raynaud’s phenomenon, which occurs in about one-third of Sjogren’s patients.
- Triggered by cold or emotional stress
- Most commonly affects fingers and toes
- Can be painful or tingly as blood flow returns
Raynaud’s is often seen in autoimmune diseases and is an important clue when combined with other symptoms.
12. Abnormal Blood Counts
Blood tests in Sjogren’s can reveal cytopenias, or low blood cell counts, in roughly half of patients:
- Low red blood cells (anemia)
- Low white blood cells (leukopenia)
- Low platelets (thrombocytopenia)
These changes may not cause obvious symptoms at first and are sometimes simply monitored. However, they are valuable indicators of disease activity and help guide treatment decisions.
13. Higher Risk of Lymphoma
One of the most serious complications of Sjogren’s is an increased risk of lymphoma, especially non-Hodgkin’s lymphoma. About 5% of patients will develop this cancer. Warning signs include:
- Persistent, enlarged lymph nodes (glands)
- Unexplained fevers
- Night sweats
- Unintentional weight loss
- New lumps or swelling that don’t go away
Any of these symptoms should be promptly reported to your healthcare provider.
How Sjogren’s Syndrome Is Diagnosed
Diagnosing Sjogren’s involves more than a single blood test. Doctors typically look at:
- Blood tests for autoantibodies such as SSA (Ro) and SSB (La)
- Other markers of inflammation or autoimmunity
- Salivary gland biopsy (small tissue sample) to look for characteristic inflammation
- Imaging, such as ultrasound of salivary glands, to assess structure and function
- Clinical symptoms, including dryness, fatigue, joint pain, and organ involvement
Not everyone with Sjogren’s has positive SSA/SSB antibodies. A skilled rheumatologist considers the full picture—symptoms, exam findings, imaging, and labs. In some cases, if antibodies are present but symptoms are mild or unclear, a “watchful waiting” approach may be recommended while monitoring over time.
Final Thoughts
Sjogren’s syndrome is a complex autoimmune disease that can begin quietly with subtle dryness or fatigue and eventually involve many parts of the body—joints, skin, nerves, lungs, and more.
If you notice persistent or unexplained symptoms like dry eyes, dry mouth, joint pain, rashes, or chronic fatigue, it’s important not to ignore them. Early recognition, evaluation by a rheumatologist, and appropriate treatment can significantly improve quality of life and help prevent serious complications.
Source: Insights adapted from Dr. Micah Yu