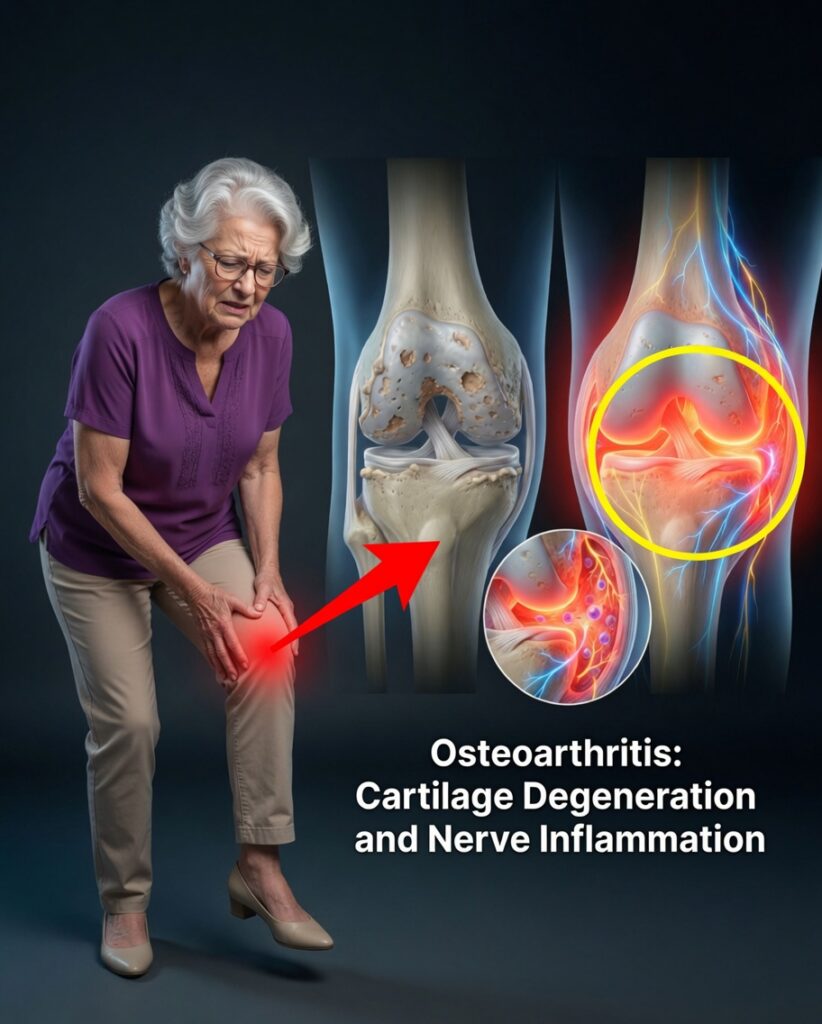
Rethinking Osteoarthritis: You’re Not Doomed to Joint Pain
Have you ever walked out of a doctor’s appointment feeling crushed after hearing you have osteoarthritis—like you were just given a lifelong sentence of pain and stiffness? Maybe someone told you, “That’s just aging, you’ll have to live with it,” or, “You’re heading toward a joint replacement.”
If you’re in your 40s, 50s, or 60s and suddenly feel decades older than you are, don’t lose hope. The full story about osteoarthritis is much more encouraging—and it’s not simply about getting old.
Osteoarthritis is commonly described as “old joints wearing out,” but that’s an oversimplification. It’s actually an active, metabolic condition influenced by inflammation and oxidative stress—factors you can often change. With the right strategy, its progression can be slowed, and in many cases, symptoms can improve.
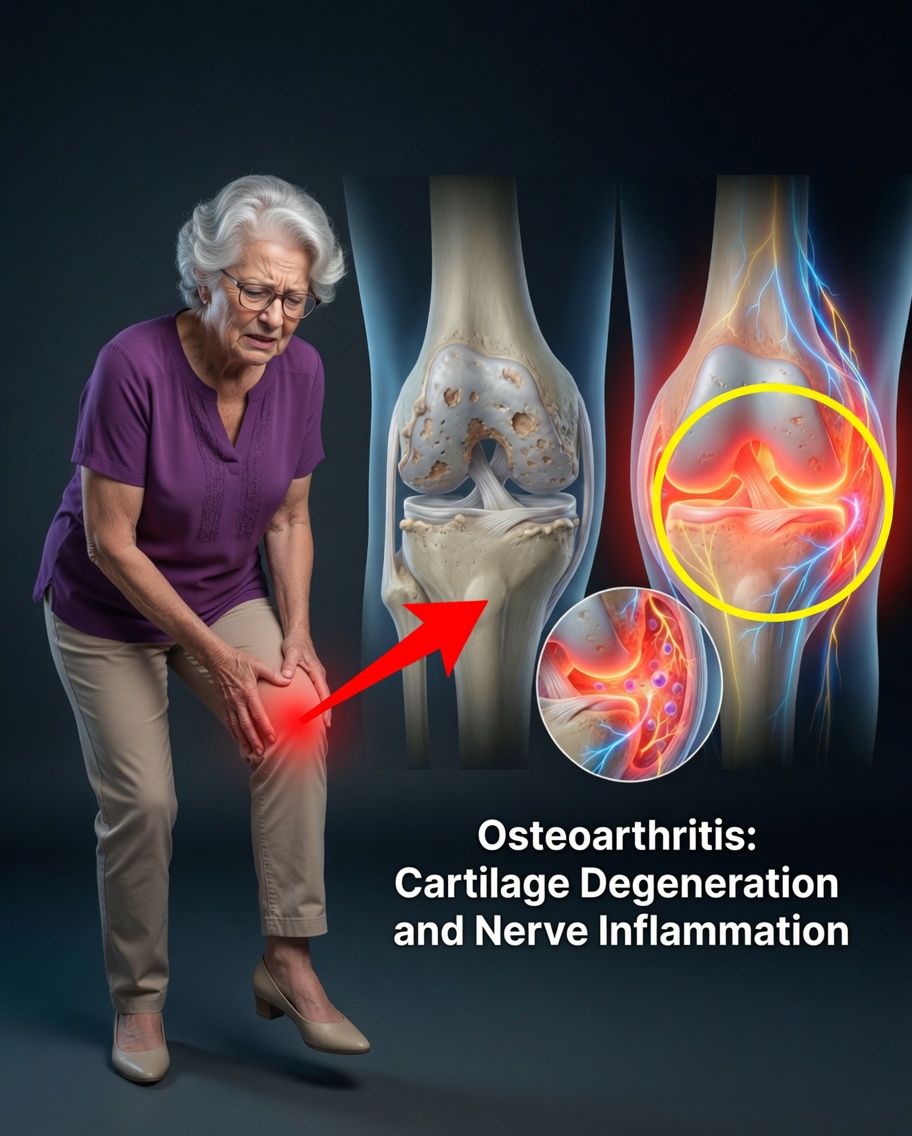
Let’s clear up the myths and focus on what truly matters when it comes to managing osteoarthritis.
Key Takeaways About Osteoarthritis
- Osteoarthritis is more than just wear and tear. It’s driven by ongoing metabolic processes and oxidative stress in the body.
- Pain doesn’t come from cartilage itself. It usually arises from inflammation and surrounding joint structures.
- Lifestyle interventions really matter. Movement, nutrition, stress management, and the right supplements can support joint health.
- Medication and surgery are not your only choices. There are proactive, practical steps you can start using now.
1. Osteoarthritis Is Not Simply “Wear and Tear”
You’ve probably heard, “Your joints hurt because you’re getting older.” That explanation is incomplete.
Osteoarthritis (OA) is better understood as an active, ongoing process involving low-grade inflammation and oxidative stress. In other words, what’s happening inside your body—your metabolism, diet, stress levels, and overall health—plays a major role.
Age alone does not dictate whether you will develop painful osteoarthritis or how severe it will be.
2. Joint Pain Comes from Inflammation, Not From Cartilage Itself
Cartilage—the smooth tissue that cushions the ends of your bones—does not contain nerves. That means it cannot directly “feel” pain.
The pain you experience with osteoarthritis usually comes from inflamed tissues around the joint, such as:
- The joint capsule
- Ligaments and tendons
- Surrounding muscles
- Bone underneath the cartilage
When these tissues become irritated and inflamed, they send pain signals—even if the cartilage damage isn’t extreme.
3. The Degree of Cartilage Damage Doesn’t Always Match the Pain
Many people are shocked to learn that:
- Some individuals have significant cartilage loss visible on imaging but little or no pain.
- Others show only mild degeneration on scans yet experience intense joint pain.
Why the mismatch? Because inflammation and sensitivity of surrounding tissues influence pain more than the exact amount of cartilage wear.
Managing inflammation and improving the health of the entire joint environment can often reduce pain, even when structural changes remain.
4. Body Weight Is Only Part of the Equation
Extra weight does put additional load on weight-bearing joints like the knees and hips. However, weight by itself is not the only driver of osteoarthritis pain.
What matters just as much—or more—is what’s happening metabolically:
- High blood sugar and insulin resistance
- Diets loaded with processed foods and added sugars
- Chronic, low-grade inflammation
Simply losing weight without addressing these factors may not fully relieve symptoms. On the other hand, improving metabolic health can significantly reduce joint irritation, even without dramatic weight loss.
5. Movement Is Medicine for Osteoarthritis
Avoiding movement out of fear of “wearing out” your joints can actually make things worse.
Cartilage has no direct blood supply. It receives nutrients through compression and decompression—in other words, through movement. Gentle, consistent motion:
- Helps nourish cartilage
- Maintains flexibility and mobility
- Strengthens muscles that support the joint
- Reduces stiffness and pain over time
Low-impact activities such as walking, swimming, cycling, yoga, and mobility exercises are often ideal for people with osteoarthritis.
6. Not All Collagen Supplements Are Equally Useful
Collagen is heavily marketed for joint health, but there’s a catch: most collagen molecules are large and not easily absorbed in their intact form. Many powders and capsules are broken down in the gut and may not directly rebuild your cartilage.
Instead of relying solely on generic collagen supplements, consider:
- Natural collagen sources like homemade bone broth
- Vitamin C, which is essential for collagen synthesis
- Omega-3 fatty acids from fish, flax, or algae, which support anti-inflammatory pathways
These combined strategies may offer more realistic support for joint health.
7. Your Diet Has a Major Impact on Joint Health
Osteoarthritis isn’t only about what you take—it’s also about what you avoid. Diets high in:
- Refined carbohydrates (white bread, pastries, sugary drinks)
- Industrial seed oils and trans fats
- Highly processed packaged foods
can increase oxidative stress and inflammation, both of which are closely linked to osteoarthritis.
For healthier joints, focus on:
- Whole, unprocessed foods
- High-quality proteins (fish, poultry, legumes)
- Healthy fats (olive oil, avocado, nuts, seeds)
- Plenty of vegetables and some low-glycemic fruits
Many people also benefit from reducing or avoiding:
- Excess gluten-containing grains
- Dairy casein (for those sensitive to it)
- Added sugar
- Alcohol
This kind of anti-inflammatory eating pattern supports the metabolic environment your joints need to function better.
8. Chronic Stress Can Accelerate Joint Breakdown
Long-standing mental or emotional stress keeps your stress hormones—especially cortisol—elevated. Over time, excess cortisol can contribute to the breakdown of joint tissues and worsen inflammation.
Supporting your nervous system is therefore part of supporting your joints. Helpful strategies include:
- Prioritizing relaxation and downtime
- Breathing exercises, meditation, or mindfulness
- Gentle outdoor activity and exposure to natural light
- Setting boundaries to reduce chronic stressors where possible
When your stress response is calmer, your body is in a better position to repair and maintain joint structures.
9. Deep, Restorative Sleep Is When Joints Repair
Most of your body’s repair and regeneration happens while you sleep, not while you’re rushing through your day. This includes joint tissues.
Aiming for about eight hours of quality sleep in a dark, quiet, cool environment can:
- Support tissue repair and collagen formation
- Lower inflammation and oxidative stress
- Improve pain tolerance and resilience
In many cases, good sleep hygiene is more powerful than any supplement for long-term joint recovery.
10. Advanced Therapies Exist—but They’re Not Standalone Solutions
There are modern, regenerative treatments that can assist in osteoarthritis management, including:
- Prolotherapy – injections aimed at stimulating tissue repair
- Platelet-Rich Plasma (PRP) – using your own platelets to promote healing
- Stem cell therapies – using stem cells to potentially regenerate damaged tissues
- Ozone therapy – sometimes used to modulate inflammation and support healing
These interventions should always be done under qualified medical supervision. They may enhance recovery, but they work best when combined with lifestyle changes, not as a replacement for them. Diet, movement, stress, and sleep still form the foundation.
Final Thoughts: You Have Real Influence Over Your Joint Health
Osteoarthritis is not an automatic, irreversible decline into constant pain and disability. While you can’t turn back the clock, you can influence:
- How quickly the condition progresses
- How much pain you feel
- How well you move and function day to day
By focusing on:
- Regular, appropriate movement
- Anti-inflammatory, nutrient-dense nutrition
- Stress reduction and nervous system support
- Quality sleep
- Thoughtful, evidence-informed supplementation and therapies
you create a powerful environment for your joints to function as well as they can.
There is no single magic pill—but small, consistent changes in your daily routine can lead to major improvements in how you feel. Instead of resigning yourself to painkillers or planning for surgery as your only option, use knowledge and action to take back control of your joint health and your future.
Source: Javier Furman